From the Editors
In the past 40 years the U.S. has experienced a dramatic shift away from large congregate care facilities to home and family-based services for people with intellectual, developmental, and other disabilities needing supports. As a result of decades of advocacy and self-advocacy, today people with disabilities have a legal right to be included in their communities. However, that right is bumping up against limitations in the systems of services and supports necessary to meet the needs of a growing population of individuals with disabilities.
In this Impact we examine some of the workforce problems in our long-term care system and their consequences for people with disabilities, the direct support workforce, families, provider agencies, and communities. We share personal stories of what is and isn’t working for those delivering and receiving supports. We look at creative, bold actions being taken around the country to address those problems. And we look at ways to be a collective force for change and ensure that quality supports are there for people with disabilities in all our communities.
Impact • Volume 31, Number 1 • Winter/Spring 2018
Managing Editor: Vicki Gaylord
Issue Editors:
Amy Hewitt, Director, Research & Training Center on Community Living (RTC-CL) Institute on Community Integration, University of Minnesota
Joseph Macbeth, Executive Director, National Alliance for Direct Support Professionals
Barbara Merrill, CEO, ANCOR
Barbara Kleist, Project Director, RTC-CL
Graphic Designers: Sarah Hollerich, Connie Burkhart
Web Developers: Shawn Lawler, Jonathon Walz, Kristin Dean
Impact is published by the Institute on Community Integration (UCEDD), and the Research and Training Center on Community Living and Employment (RTC), College of Education and Human Development, University of Minnesota. It is supported, in part, by Grant #90DD0001 from the Administration on Intellectual and Developmental Disabilities, US Department of Health and Human Services (HHS), to the Institute; and Grant #90RT5019 from the National Institute on Disability, Independent Living, and Rehabilitation Research (NIDILRR), HHS, to the RTC. Additional support for this issue was provided by Grant # T73MC12835 from U.S. Department of Health and Human Services(HHS), Maternal and Child Health Bureau, to the Minnesota LEND.
The views expressed are those of the authors and do not necessarily reflect the views of the Institute, Center or University. The content does not necessarily represent the policy of the US Department of Health and Human Services, and endorsement by the Federal Government should not be assumed.
For print copies contact: Institute on Community Integration, University of Minnesota, 109 Pattee Hall, 150 Pillsbury Dr. SE, Minneapolis, MN 55455 • 612/624-4512 • icipub@umn.edu.
Impact is available in alternate formats upon request. The University of Minnesota is an equal opportunity employer and educator.
On the cover: Walter Gill’s experiences receiving support, and Sara Stockdale’s experiences as a Direct Support Professional, are among the stories in the upcoming book, A Community Life: Community Living and Participation for Individuals with Intellectual and Developmental Disabilities published in fall 2018 by AAIDD.
overview
The Direct Support Workforce Crisis:
A Systemic Failure

Around the country people are pushing for changes that address the direct support workforce crisis. Among them are those rallying in New York City (pictured here). Photo courtesy of BFair2DirectCare.
Direct Support Professionals (DSPs) provide daily support to people with intellectual and/or developmental disabilities (IDD) so they can live and participate in their communities as friends, neighbors, coworkers, students, family members, volunteers, voters, and taxpayers. Increasingly these supports are provided inside the individual or family home, allowing other family members to work and have respite from their daily caregiving. Individuals with IDD and their families rely heavily on the direct support workforce to be reliable, stable, and competent.
The reality is that significant challenges remain in finding, keeping, and training DSPs who support persons with IDD, and these challenges — often labeled a "crisis" — have plagued this industry since the inception of community services. A 30-year crisis is not a crisis; it is a systematic and pervasive failure in the long-term services and supports system in the United States that has created a public health crisis. This failure is rooted in the tacit acceptance that, although not ideal, intense competition for public funding seems to translate to a relatively low-wage workforce and "adequate" services for people with disabilities. That acceptance must be challenged and labeled as what it is: a fundamental lack of respect for people with disabilities and the staff who choose careers in providing support to them.
The Direct Support Workforce
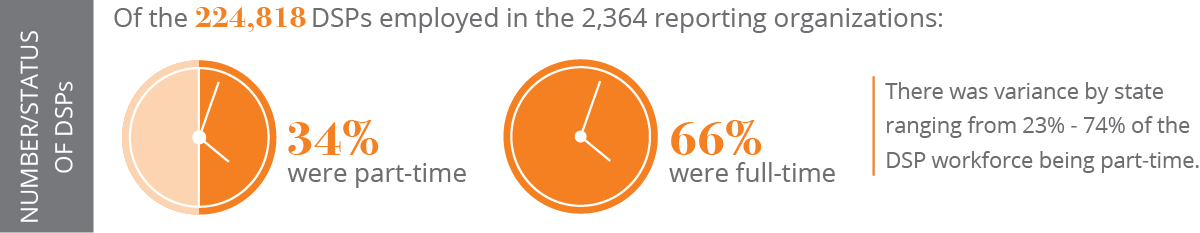
Direct Support Professionals are the paid staff who support individuals with IDD to live their lives and enjoy the same opportunities and experiences as people without disabilities. DSPs support people in whatever ways they need to enhance inclusion and independence. These workers are employed in many types of settings, including family/individual homes, intermediate care facilities, small community residential group homes, community job sites, vocational and day training programs, and others. The direct support workforce includes full-time (66%) and part-time (34%) employees (NCI, 2018). Most employers use the occupational title of Direct Support Professional, yet many DSPs may have different titles including direct support specialist, personal care assistant, habilitation specialist, job coach, residential counselor, family care provider, personal assistant, and others.
A 30-YEAR CRISIS IS NOT A CRISIS; IT IS A SYSTEMATIC AND PERVASIVE FAILURE IN THE LONG-TERM SERVICES AND SUPPORTS SYSTEM IN THE UNITED STATES THAT HAS CREATED A PUBLIC HEALTH CRISIS.
The workforce is predominately made up of women (89%) (PHI, 2011; Hewitt et al., 2008) with an average age of 42 years (PHI, 2011). About 50% of direct support workers rely on means-tested public assistance (Espinoza, 2017). The direct support workforce is racially and ethnically diverse, with 47% of the workforce being white (non-Hispanic), 30% African American, 16% Hispanic/Latino, and 7% other (PHI, 2011). Nearly one-fourth of the direct support workforce was born in a country other than the U.S., compared to 16% of the total U.S. workforce (BLS, 2016). About 45% of direct support workers have completed some college coursework or have a college degree.
Size of the Direct Support Workforce
No occupational title of Direct Support Professional is currently recognized by the Bureau of Labor Statistics (BLS). DSPs are identified within three primary Standard Occupational Classifications of the U.S. Department of Labor: (1) Personal Care Assistant, (2) Home Health Aide, and (3) Nursing Assistant. In 2015 there were roughly 4.5 million direct support workers categorized within three occupational categories (Espinoza, 2017; BLS, 2015). Given the range and variation of job titles assigned to DSPs who work for people with an IDD, some may be miscounted, undercounted or not included in the current BLS classification.
Based on estimates from state-specific studies reporting the number of people who receive services and staffing ratios it is possible to make reasonable estimates of the size of the DSP workforce that specifically supports people with IDD. Recent estimates suggest that in 2013 there were about 880,000 full-time equivalent (FTE) DSP positions dedicated to providing assistance to 1.4 million people. Given that approximately 30% of the DSP workforce is part-time, and estimating that 2.5 part-time workers are needed to fill one full-time equivalency, there were an estimated 1,276,000 DSPs supporting individuals with IDD on June 30, 2013. In order to be able to sustain services at the current levels, given current turnover rates, every year 574,200 new DSPs need to be hired into the workforce. To provide services to the approximately 200,000 people with IDD on waiting lists, an additional 167,001 new DSPs would need to be hired. Given the high growth and demand in need for long-term services and supports, the persistent turnover rates, and a strong U.S. economy, the number of new DSPs that will need to enter the workforce is expected to grow each year between now and 2030.
What DSPs Do
In many ways, DSPs are generalists who have to be able to provide whatever support is needed across a wide range of activities throughout the lifespan of people with IDD. They provide support that promotes informed decision making, understanding risk, exercising rights and choices — empowering people by teaching, modeling, and supporting them in all aspects of life. DSPs implement support for health and wellness routines such as dispensing medications and implementing significant treatments and medical interventions. DSPs assist at medical appointments where they support people with IDD to communicate and interact with a variety of medical professionals about health-related issues. Effective DSPs must monitor for emerging signs and symptoms of illness or disease, and be attentive and energetic in promoting healthy lifestyles. On a daily basis, many DSPs provide assistance for all types of daily living skills, and support the use of assistive technology devices for communication and mobility. Aside from residential supports, DSPs help people find and keep jobs. Of critical importance, DSPs support people by promoting healthy relationships with family, friends, and co-workers. They get people socially connected and support them to participate in social and spiritual activities, education, cultural events, and community functions.
The direct support job is highly complex and requires sound judgment and significant skills that include independent problem-solving, decision-making, behavioral assessment, crisis prevention and intervention, and communication. Many DSPs are often isolated, without co-workers, supervisors or clinical professionals on-site to provide assistance or guidance. DSPs are interdisciplinary professionals because their job duties resemble many tasks typically completed by teachers, nurses, allied health professionals, social workers, counselors, and others. Highly effective DSPs are skilled at developing strong relationships with those they support and their families, and are flexible enough to change depending on each person’s needs and abilities.
Pervasive Workforce Challenges
The direct support workforce is large and is one of the highest-demand and anticipated growth areas in the U.S. Expansion of this workforce is not possible without significant improvements in how they are recruited, on-boarded, and developed. Low wages, unaffordable benefits, limited training and development, and lack of career advancement opportunities make this work undesirable for many people. These challenges impact individuals, families, and community providers who are finding it increasingly difficult, if not impossible, to find and keep high quality employees.

Wages and Benefits
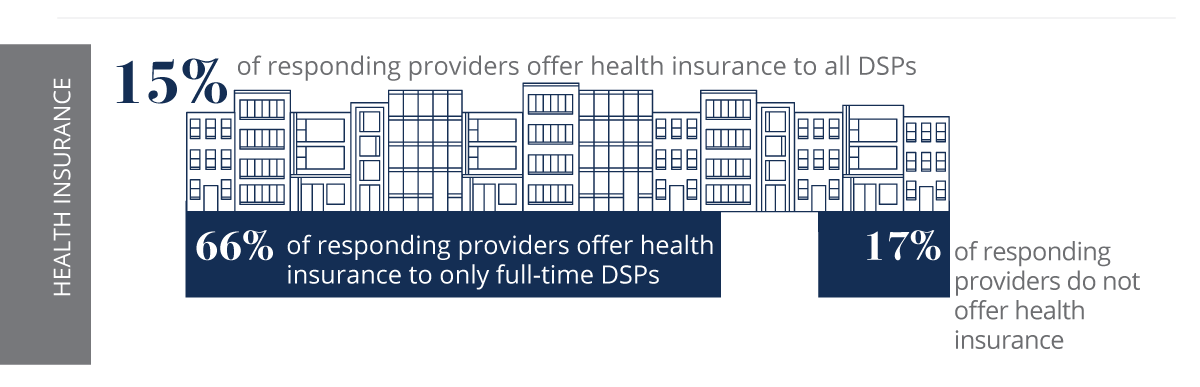
The national average wage for DSPs is $11.76 per hour (NCI, 2018). This workforce has actually seen their wages decline over time when wages are adjusted for inflation (PHI, 2015). At $11.76, the average DSP who works full-time makes below the federal poverty level for a family of four (HHS, 2017). Many organizations provide health insurance to employees, but it is far too common that DSPs do not utilize what is offered because they cannot afford the premiums. Most organizations offer paid time off to full-time DSPs, but often part-time workers have no paid benefits. Almost half of DSPs receive publicly-funded benefits, such as medical, food or housing assistance (PHI, 2015). Most DSPs work a second (or third) job to earn enough money to pay their bills (Test, Flowers, Hewitt, & Solow, 2003). Unacceptably low wages and limited benefits result in recruitment and retention challenges for organizations who hire DSPs.
High Turnover and Vacancy Rates
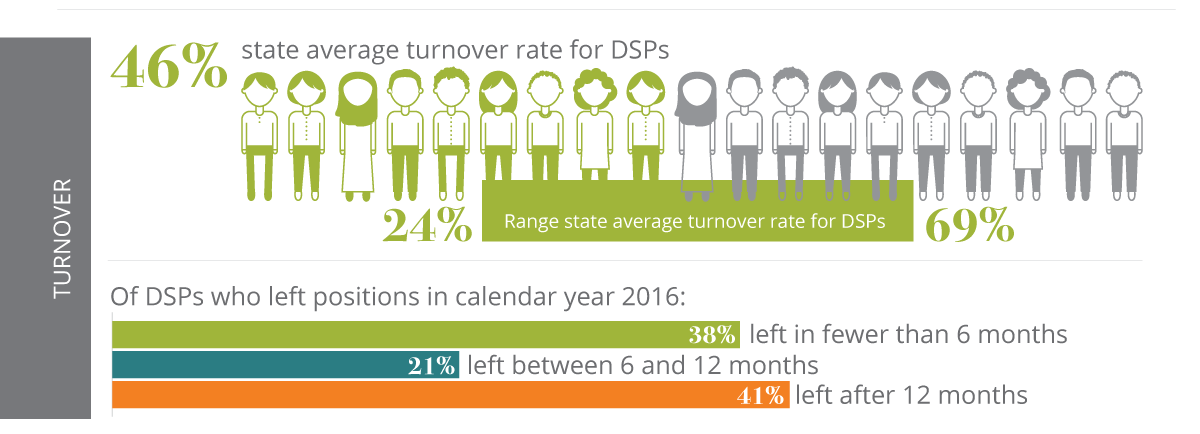
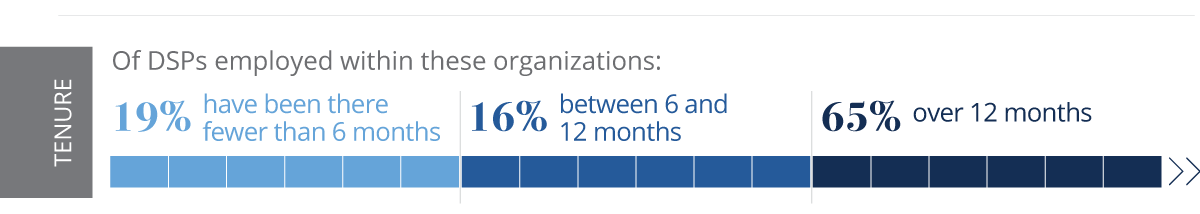
High turnover has been well documented in the DSP workforce for nearly three decades (Bogenshutz, Hewitt, Nord, & Hepperlen, 2014; Braddock & Mitchell, 1992; Larson, Lakin & Bruininks, 1998; Larson, Hewitt, & Knoblauch, 2005; ANCOR, 2010; Hewitt, Taylor, Kramme, Pettingel, & Sedlezky, 2015). The average annual turnover for DSP positions is an estimated 46%, with a range of 24–69% (NCI, 2018). About 38% of DSPs leave their positions in less than six months, and approximately 21% leave within 6–12 months. Across all industries, the national average separation (turnover) rate is 3.5% (BLS, 2017). Costs associated with replacing DSPs in IDD services range between $2,413 and $5,200 (Hewitt & Larson, 2007; ANCOR, 2010; Medisked Connect, 2016). Using a conservative number, the costs associated with turnover are substantial. In New York state, for example, the cost of replacing DSP workers, using an average cost per person of $4,073, was estimated at $79,804,549 in 2015 (Hewitt et al., 2015). Workforce insufficiency is also seen in high vacancy rates; current vacancy rates within long-term services and supports for people with IDD are more than 9% (Hewitt et al., 2015; Hiersteiner, 2016).
THERE ARE MANY EXAMPLES OF PROMISING PRACTICES THAT, IF TAKEN TO SCALE THROUGHOUT THE U.S., COULD LEAD TO MUCH-NEEDED CHANGE.
Training and Career Development
Direct Support Professionals need better training. Most do not come to their jobs with the knowledge, skills, and attitudes required of their roles. Federal regulations are largely silent about the preservice and in-service training required for DSPs to provide quality community support to people with IDD. At a state level it is often common that employers are required to provide a minimal number of preservice training hours (around 40) that focus on topics or basic skills that must be taught within a certain number of hours post-hire (e.g., CPR, first aid, documentation, blood-borne pathogens) and at regular intervals after hire. Rarely is engaging, interactive, competency-based training required or expected. Yet, we know far too well that research-based knowledge, sophisticated skills, and high ethical standards are required of DSPs to be effective in their jobs. Over the past several decades many sets of national and state DSP-specific competencies have been identified and refined.
Quality Long-Term Services and Supports Are Not Possible Without Quality Staff
Direct Support Professionals deliver the support needed for individuals to achieve their personally desired outcomes. This was recently acknowledged by the National Quality Forum (NQF, 2016) in their home and community based services (HCBS) quality framework. Within this framework the direct support workforce was identified as a key quality domain including a focus on the following: (1) DSPs have a person-centered approach to services; 2) DSPs have demonstrated competencies; (3) the organization and state ensure safety and respect for the worker; (4) there are sufficient workforce numbers, dispersion, and availability; (5) DSPs are adequately compensated with benefits; (6) DSPs are culturally competent; and (7) DSPs are engaged and participate in the organization and system (NQF, 2016). An increasing number of states are paying attention to the need to know more about their direct support workforce. As a result, National Core Indicators (NCI) created a staff stability survey, which is currently being used in 20 states and the District of Columbia, and obtains information about turnover and vacancy rates as predictors of individual outcomes (NCI, 2018).
Heavy Consequences
The ongoing systemic and pervasive failures in the long-term services and supports system have created heavy consequences for DSPs, individuals with IDD, families, organizations, and businesses, including the following:
- Direct Support Professionals. High turnover rates result in many DSPs being overworked, tired, and more prone to making mistakes. That coupled with the economic stresses of their employment can undermine the willingness of DSPs to remain in their jobs. Many DSPs are able to stay in the direct support workforce because they are willing to work two or three jobs and 80 hours a week to have enough income to support their families. Low wages often correlate with low value, respect, and status. DSP wages are so low and their accountability so high, that far too often good people leave a highly skilled profession they love.
- Individuals with Intellectual and/or Developmental Disabilities. The health, safety and well-being of people with IDD is at risk daily because of the workforce problems. A revolving door of strangers coming in and out of a person’s life, often required to support in the most intimate personal care routines, means that far too often they may not trust or develop a meaningful professional relationship with the DSP. Signs and symptoms of illness are missed, opportunities for community participation are lost, and people with an IDD have few choices other than congregate models, such as group homes or sheltered work settings, because community staffing is unstable.
- Families. Having skilled, committed, and known direct support providers is critical for family members to maintain employment and engage in their own community life. More than half of parents interviewed reported major career concessions (e.g., not taking a job, working fewer hours, dropping out of the workforce, turning down a promotion) related to having a child with IDD (Anderson, Larson, Lakin, & Kwak, 2002). Family members report they find it challenging to get any respite and this causes stress, health issues, burnout and, ultimately, added societal costs.
- Organizations and Businesses. The costs and wasted resources associated with high DSP turnover over decades has resulted in serious consequences for providers. This sustained turnover rate alone is debilitating; when coupled with low unemployment rates across industries since the Great Recession, organizations simply cannot find enough qualified individuals to fill positions. The limited candidate pool, and greater competition from other businesses and industries that pay better wages, have resulted in organizations being forced to consider applicants they would not have previously hired. This "lowering of the bar" results in less dependability among DSPs, and an increase in unacceptable workplace behavior among some employees (e.g., theft, drug use, neglect/abuse, unethical behavior, poor decision-making).
Conclusion
Solutions to the direct support workforce crisis are critical to ensuring that people with IDD can live, work, and contribute in their communities. Such solutions are also important because of the significant economic implications. There are many examples of promising practices that, if taken to scale throughout the U.S., could lead to the much-needed change and comprehensive systems solutions. Such solutions have the potential to promote job growth and development by filling critical vacancies and supporting growth in this industry. They will bring about greater use of public resources through cost-effective savings created by reducing the costs associated with high turnover. They will allow family members of people with IDD to keep jobs and accept promotions, increasing families’ economic well-being. Lastly and most importantly, finding solutions will improve the quality of supports and services for people with IDD and increase their full participation in community life.
These much needed solutions will not be easy and will most certainly require enormous amounts of focused advocacy and energy by people with IDD, families, allies, and advocates. But, the time for acceptance of constant crisis and a flawed system has passed. We need to boldly force solutions now!
References
- American Network of Community Options and Resources (ANCOR). (2010). 2009 direct support professionals wage study. Alexandria, VA: Author.
- Anderson, L.L., Larson, S.A., Lakin, K.C., & Kwak, N. (2002, August). Children with disabilities: Social roles and family impacts in the NHIS-D. DD Data Brief, 4(1). Minneapolis: University of Minnesota, Institute on Community Integration.
- Bogenshutz, M.D., Hewitt, A., Nord, D., & Hepperlen, R. (2014). Direct support workforce supporting individuals with IDD: Current wages, benefits, and stability. Intellectual and Developmental Disabilities, 52. 317-329. doi:10.1352/1934-9556-52.5.317
- Braddock, D., & Mitchell, D. (1992). Residential services and developmental disabilities in the United States: A national survey of staff compensation, turnover and related issues. Washington D.C.: American Association on Mental Retardation.
- Bureau of Labor Statistics (BLS), U.S. Department of Labor. (2017, April). Job openings and labor turnover — February 2017. (News Release USDL-17-0416).
- Bureau of Labor Statistics (BLS), U.S. Department of Labor (2016, May). Labor force characteristics of foreign-born workers summary. (News Release USDL-16-0989).
- Bureau of Labor Statistics (BLS), U.S. Department of Labor. (2015, December). Fastest growing occupations. Occupational Outlook Handbook.
- Espinoza, R. (2017). Federal policy priorities: Strengthening the direct care workforce. Bronx NY: Paraprofessional Healthcare Institute [PHI].
- Hewitt, A., & Larson, S. (2007). The direct support workforce in community supports to individuals with developmental disabilities: Issues, implications, and promising practices. Developmental Disabilities Research Reviews, 13, 178-187. doi:10.1002/mrdd.20151
- Hewitt, A., Larson, S., Edelstein, S., Seavey, D., Hoge, M.A., & Morris, J. (2008). A synthesis of direct service workforce demographics and challenges across intellectual/developmental disabilities, aging, physical disabilities, and behavioral health. Minneapolis: University of Minnesota, Institute on Community Integration, Research and Training Center on Community Living.
- Hewitt, A., Taylor, M., Kramme, J., Pettingel, S., & Sedlezky, L. (2015). Implementing direct support professional credentialing in New York: Technical report. Minneapolis: University of Minnesota, Institute on Community Integration, Research and Training Center on Community Living.
- Hiersteiner, D. (2016). National core indicators: 2015 Staff stability survey report. Cambridge, MA: Human Services Research Institute and The National Association of State Directors of Developmental Disabilities Services, Inc.
- Larson, S., Hewitt, A., & Knoblauch, B. (2005). Recruitment, retention, and training challenges in community human services: A review of the literature. In S. Larson & A. Hewitt (Eds.), Staff recruitment, retention, and training strategies for community human services organizations (pp. 1-18). Baltimore, MD: Paul H. Brookes.
- Larson, S., Lakin, K.C., & Bruininks, R. (1998). Staff recruitment and retention: Study results and intervention strategies. Washington, DC: American Association on Mental Retardation.
- Medisked Connect. (2016). The staffing struggle is real: New statistics on I/DD agencies’ most common staffing problems + 5 tips for reducing employee turnover.
- National Core Indicators (NCI). (2018, February). 2016 Staff stability survey.
- National Quality Forum (NQF). (2016). Quality in home and community-based services to support community living: Addressing gaps in performance measurement. Washington, D.C.
- Paraprofessional Healthcare Institute (PHI). (2015). Paying the price: How poverty wages undermine home care in America. Washington, D.C.: Author.
- Paraprofessional Healthcare Institute (PHI). (2011, February). Who are direct-care workers? PHI Facts. Washington, D.C.: Author.
- Test, D.W., Flowers, C., Hewitt, A.S., & Solow, J. (2003). Statewide study of the direct support staff workforce. Mental Retardation, 41, 276-285. doi:10.1352/0047-6765(2003)412.0.CO;2
- U.S. Department of Health and Human Services (HHS). (2017). Annual update of the HHS poverty guidelines. 82 Fed. Reg. 8831.
- U.S. Department of Health and Human Services (HHS). (1996). Opportunities for excellence: Supporting the frontline workforce. Washington, D.C.: President’s Committee on Mental Retardation.
personal story
“We’re Talking About Lives Here”
The Personal Impact of the Direct Support Workforce Crisis

Shawn (left) and Jim are navigating the challenges of direct support, including understaffing for Shawn and a path to burnout for Jim.
Shawn is a young man with a disability for whom direct support is essential, not only for his physical well-being, but also for his participation in his community. Jim is a Direct Support Professional (DSP) who has supported Shawn for four years and whose commitment to direct support — and Shawn — has made a big difference in both their lives. They were interviewed in fall of 2017 and asked to talk about the DSP workforce crisis and how it affects them. Below are their reflections.
- Shawn
- I've known Jim for four years now and he helps me every weekday morning — he's my daytime staff — with things like getting dressed, getting meals, helping me in the bathroom, that sort of thing. And then we go out and do activities, like I work out a couple times a week or go hit a mall for walking or shopping, those sorts of things.
- Jim
- Like Shawn said, I've been with him for four years. This is self-direction, and it's really cool stuff. I enjoy it — we're out in the community, we're on the go. Shawn does not like to sit around, he likes to go. He’s very, very busy, which sometimes can be a little bit challenging for me. With him being so busy and me trying to keep up with my schedules of stuff that I do, it's been a challenge, but it's been a wonderful thing. The self-direction program, I believe, is going in the right places. It's just a great thing for Shawn. He's been doing some boxing, he's been doing a little bit of weight lifting, he does skiing…
- Shawn
- I've been playing sled hockey for three years.
- Jim
- Overall, it's a wonderful thing. We’re in rallies all the time for Be Fair to Direct Care [a grassroots campaign in New York state to get to a living wage for the direct support workforce]. We are constantly fighting for wages for everyone.
- Shawn
- The reason Be Fair to Direct Care got started is the base salary for people like Jim who are DSPs is just, honestly, too low to attract the quality of workers that we need and we are constantly under-staffed. I have not been fully staffed for the last four years. I make it work through family and friends, but I've not had all my hours covered in four years. The base salary right now stands at $10.20; because of the increase in minimum and the Be Fair to Direct Care money from last year, that will jump to $10.75 by January 1st. Which is still too low to attract the quality of people that we need when they can get better paying jobs elsewhere.
- Jim
- It seems to be such a complicated thing for the senate to get these funds passed. I don't know why, it's a no brainer. These are people who really need quality care and if we don't attract people to come work with decent wages, we're never gonna get it. Constantly we're down on numbers. I'm running like 60, 80 hours a week of overtime. The overtime has been tremendous and that's the only way that I can survive. I am working between 60 and 80 hours of overtime, and this has been a constant since I've been here for the last four years. I'm trying to survive in this field and I'm trying to take care of the people that I enjoy working with, being with. And it's just been a big battle and they seem to ignore us, they seem to want to ignore us. I don't know why, because we're talking about lives here. The dropout rate — they get hired, then they quit. We need to attract better, more qualified people and that's gonna come with better wages.
- Shawn
- One time Jim and I did the math just for his basic expenses of apartment, gas, electric, and he could not survive without overtime.
- Jim
- I could never survive without over-time. It's pretty sad that I feel like, honestly, I feel like I'm on a slow death trend because of the constant overtime. It's called burnout, and it plays a big part for me, being an older gentleman now. But I'm experienced, so I kind of know how deal with it and keep myself going. But it's really sad.
- Shawn
- I mean, Jim has approximately 20 years of experience and his base pay rate is $11 an hour.
- Jim
- Now you figure overtime is $16.50, you know.
- Shawn
- Because they pay time-and-a-half.
- Jim
- And then I'm working 60 to 80 hours for, you know, maybe a couple thousand dollar paycheck. That's a lot of hours and yes, I need that money to survive. This is all I have, this is my last stop, I don't want to go on to any other place. I love what I do. These guys and gals are my life. I don't have a personal life and it's really starting to settle in on me, and I'm saying okay, I got to slow down, I got to spend more quality time at my home with my kids and my girlfriend and so forth. It’s hard to hold onto relationships when you're always working.
- Shawn
- And then on my end of things, as I mentioned, I have not been fully staffed in four years. So there are points in my schedule where I'm supposed to have coverage and I don't, so I end up falling back on my family to provide that care that's supposed to be covered by the agency. And sometimes that causes issues, sometimes I may have to cancel something that I had planned simply because I don't have staff to cover it. I am lucky that my family supports me very well and will step in and do the basic care that my aids take care of so that I'm not sitting in my own filth for any period of time; they will take care of that sort of thing. But I am fortunate, and not everyone has those back-up supports.
- Jim
- I consider Shawn in the fam, and Mary [Shawn’s life partner], and Phred [the nickname for Mary’s mother], and Bobby, who's his nephew. I'm always there, and we work together if something can't get covered. Mary and I will work it out where, you know, I can get a little time to go to the doctor's appointment or something. We have to work together.
- Shawn
- Yes, we do. I've known Jim for four years. I consider him to be family also, and when he has a need like that, we sit down and work it out to make it happen. We have to work together or it won't work.
- Jim
- But I want to keep going. I like it and I want to keep going, but we’ve got to have better wages because, you know, I'm not getting any younger. I call it a slow death.
- Shawn
- Yeah.
overview
Here’s How We Achieve a Strong Economy:
Invest in Direct Support Workers
In the last 10 years, the long-term care industry created 1.5 million jobs (BLS, 2017a). Most of this job growth was due to the rising demand for direct support workers — personal care aides, home health aides, and nursing assistants — spurred by the growth in the population of older adults (see Figure 1). From 2016 to 2026, an additional 1.8 million jobs will be created in the long-term care sector (see Figure 2), which includes services for older adults and people with disabilities such as continuing care retirement communities, assisted living facilities, home health care services, nursing homes, residential facilities that support people with intellectual and developmental disabilities, and vocational rehabilitation services (BLS, 2017b). Those 1.8 million new jobs are projected to include 1.2 million direct support jobs.
This growing demand for direct support workers means that job creation in the U.S. will increasingly be driven by the need for hands-on support for older adults and people with disabilities. However, direct support jobs compensate workers poorly and leave many in poverty. If these issues are not addressed, growth in these jobs may contribute to greater financial instability for American families. To meet new demand for care and to ensure a strong economy, we need to improve the quality of direct support jobs.
Today, direct support workers earn a median annual income of $17,000 (PHI, 2017, Nov. 10). One in five direct support workers lives in poverty, and nearly half rely on public assistance to support their families. Home care workers face even greater financial instability than direct support workers in other industries (PHI, 2017a). Women of color in direct support are especially disadvantaged — they constitute a large and growing segment of the workforce, yet they are more likely to live in poverty than their peers (PHI, 2017b). Living wages, better training and advancement opportunities, employer-provided benefits, and full-time hours for direct support workers would help ensure that new job openings in the fastest-growing segment of our economy translate into better economic opportunities for job seekers.
New jobs in direct support will also enable workers in other sectors to participate in the economy more fully — family caregivers in the labor force will be able to reliably supplement their unpaid care by hiring direct support workers. Currently, most of the 44 million family caregivers in the U.S. have changed their work schedules or left their jobs to attend to loved ones (National Alliance for Caregiving & AARP Public Policy Institute, 2016) and these family caregiving obligations ultimately cost the economy $28 billion in lost productivity (Witters, 2011). Women in the workforce are disproportionately impacted, as women constitute two-thirds of family caregivers. Ensuring an adequate supply of direct support workers will allow other workers to reach their full economic potential with the peace of mind that their loved ones are supported.


References
- National Alliance for Caregiving & AARP Public Policy Institute (2016). Caregiving in the U.S. Washington, D.C.: AARP Public Policy Institute.
- PHI (2017a). U.S. home care workers: Key facts. Bronx, NY: PHI.
- PHI (2017b). Racial and gender disparities within the direct care workforce: Five key findings. Bronx, NY: PHI.
- PHI (2017, Nov. 10). Workforce data center
- U.S. Bureau of Labor Statistics (BLS). (2017a). Current employment statistics — CES (national): Employment, hours, and earnings. National analysis by PHI (October 4, 2017).
- U.S. Bureau of Labor Statistics (BLS). (2017b). 2016-2026 Employment projections.
- Witters, D. (2011, Dec. 1). The cost of caregiving to the U.S. economy. Gallup News.
overview
What’s Causing the Crisis?
Direct support workforce challenges have existed for decades. Many factors are influencing what many fear is an impending implosion of long-term services and supports, if solutions are not found. Among the most influential factors are:
Limited Wages, Benefits, and Career Pathways
No matter how much DSPs might love their jobs, they need to be able to support themselves and their families. Low wages and lack of affordable benefits are universally identified by agencies, DSPs, and people who receive supports as the most significant issue. In addition, career pathways do not exist for DSPs. There are no required credentials that ensure DSPs have met the knowledge requirements and demonstrated proficiency in skills needed for the job, nor to certify a person’s commitment to the profession. With few opportunities for growth and development there’s little increased earning potential, and many DSPs leave the profession.
Changing Demographics
America is aging, with an anticipated 98 million people reaching 65 years of age and older by 2060 (ACL, 2017). There is also a smaller population of young workers available to enter the labor market. With more people entering retirement years, and an overall decrease in the percentage of the population in the labor force, there is increased competition for workers across all industries — including long-term services and supports — and fewer available to fill openings. This potentially reduces the number of new entrants into the direct support workforce even as the number of people needing those services grows.
Longer Lifespans
Life expectancy for individuals with IDD has increased from an average of 19 years in the 1930s to 66 years today (Coppus, 2013), and those with mild intellectual disabilities have life expectancies similar to the general population (74 years). People with IDD are living longer because of advances in medicine and improved healthcare, better nutrition, decreases in institutionalization, and increases in community participation. When people with IDD live longer, the number of years they require services increases and creates additional demand for DSPs.
Shifts in Laws and Expectations
As the result of Section 504 of the Rehabilitation Act, the Individuals with Disabilities Education Act, the Americans with Disabilities Act (ADA), and the Supreme Court’s holding in Olmstead v. L.C. and E.W. that the "integration mandate" of the ADA requires public agencies to provide services "in the most integrated setting appropriate to the needs of qualified individuals with disabilities," people with IDD and their families have a legal right to expect to live and be included in their communities. The overwhelming majority now receive individualized supports in their homes and community instead of large congregate care facilities. The shift from congregate care to home- and family-based services demands increased skill, sophistication, and flexibility on the part of DSPs.
References
- Administration for Community Living (ACL). (2017). A profile of older Americans: 2016.
- Coppus, A.M.W. (2013). People with intellectual disability: What do we know about adulthood and life expectancy? Developmental Disability Review, 18, 6-16. doi:10.1002/ ddrr.1123
overview
The Evolving Role of DSPs:
Supporting Life Outcomes
Direct Support Professionals (DSP) fill an important role in the lives of persons with intellectual and developmental disabilities (IDD). The field has seen the evolution of this role from ensuring a person's health and safety to focusing on quality of life outcomes achieved through accessing opportunities in the community. The dedication and commitment of DSPs is a constant in our field; however, their roles continue to be redefined by the values and beliefs of person-centered, self-directed, and community-based models of supports and services.
Understanding the Past
To understand the current roles, it is important to reflect on the history of how and where supports were provided. Within institutions, DSPs were often a link to relationships with others outside of the setting through facilitating community visits or bringing community members onto the grounds. When it came to relationships with parents or families, a common practice was to "cut-off " ties in order to ease stress and emotions. Today, this may seem harsh, but the intent was to help the person with IDD and the family adjust to their new living arrangements and decrease the stress this caused.
In the early years of home and community based services, provider agencies were the sole resource for delivering needed community supports, typically through group homes, day centers, and sheltered workshops. The DSP role was to implement the policies and practices of the organization and serve as an ally to the agency. Staff who worked in group homes or day programs worked through schedules, ran programs that focused on skill building, and led people into community places. The organizational focus on health and safety was often the dominant directive, and staff interactions with families or community members were often limited. Although the mission of the organizations was about having the person be a part of the community, certain practices, schedules, and regulations created a barrier that often disconnected the person from family and community (see Figure 1, Traditional).

Traditional Disability Services
Focus has been on specialized or segregated supports that can, at times, become a barrier between the person and their chosen participation in family and community.

Integrated Services and Supports
Focus is on integrating supports into the person’s life in a way that upholds the person’s chosen involvement with family and community.

Types of Supports Leveraged
With integrated services and supports, DSPs must navigate a range of resources, relationships, and networks in the community.
In the early 2000s, expectations of support began to change as more K-12 students with IDD were completing high school alongside their peers without disabilities, and shared the same expectations of being employed, living in the community, and being active members of society. Provider organizations and state-operated agencies began to embrace person-centered practices and self-directed supports. In doing so, they recognized the need for new and innovative models for long-term services and supports that met these new expectations while building and sustaining their longstanding commitment to people with IDD (see Figure 1, Integrated).
Evolving Support Structures
Changes to the delivery of supports have brought new expectations and realities that impact every aspect of the system — state entities, provider agencies, the person being supported, the family, and DSPs. Overall, federal and state policy and guidance have been adjusted to reflect inclusive community practices, such as the Centers for Medicare and Medicaid Services’ home and community based services (HCBS) settings rule (CMS, 2014). Funded supports are being provided in a person's home (supported living) or in the home of their family (family-based support). Administrative activities, such as hiring, training, scheduling, and documentation, are being provided by either traditional provider agencies or the person with IDD themselves through self-directed options. The DSP has become an ally to the person supported while serving as a representative of the organization for which they work.
These changes have a direct impact on the roles of DSPs, both in terms of positive changes and an added level of complexity. Staff are now being matched with the person they support — recognizing personalities, interests, needs, and culture — which increases job satisfaction and improves supports. Recruitment is heavily dependent on people already known to the person, including family members, classmates, and neighbors. The person-centered plan has become the blueprint for DSPs to provide supports and focus on long-term goals. The day-to-day supports are driven by the person being supported, and delivered in the places the person chooses to go and environments where they are most comfortable.
WITH THE EMERGENCE OF INTEGRATED SUPPORTS AS A FOCUS OF THE DISABILITY FIELD AND THE ROLE OF DSPS, MORE MUST BE DONE TO TEACH THE SKILLS AND STRATEGIES NECESSARY TO MAKE THIS POSSIBLE.
Changing Expectations
DSPs are now navigating new territory. They are asked to provide supports that balance health and safety with self-determination and engagement, often without clear guidelines from many states, agencies, and families. They are asked to assure safety while acknowledging and supporting how the person sees their life within the home, culture, and community of that person. Their focus is on supporting the person, but they must acknowledge and interact with family members, friends, and neighbors. This requires DSPs to navigate the day-to-day routines, realities, relationships, and expectations of not only the person they are supporting, but of those who might be around them. While person-centered support plans offer a good understanding of what is important to and for the person, DSPs are often left without a lot of guidance on strategies for building capacity, coaching or supporting that specific person to achieve their personal outcomes.
There are many other new and competing expectations of DSPs who are working within a person-centered, community-based model, but one of the most important roles is for DSPs to assist a person to access integrated supports within the community while maintaining and building relationships with their friends and family (see Figure 1, Types of Supports). DSPs must understand and navigate formal disability supports, as well as leverage and connect to other forms of supports such as technology, relationships, and community resources. DSPs must use their own social capital and networks to connect the person to resources and people in their community that can be tapped into to achieve their desired outcomes and goals. DSPs assist the person they support in learning and using technology daily to achieve personal goals, whether it is to support taking transportation, connecting with friends or using remote monitoring for long distance support. With the emergence of integrated supports as a focus of the disability field and the role of DSPs, more must be done to teach the skills and strategies necessary to make this possible; often this is left primarily for the person, family, and DSP to navigate.
Conclusion
As DSPs assist the people they support to identify their "good life," they are providing support to keep each person on the trajectory towards that vision. New roles include such things as providing transportation, facilitating relationships with friends and peers, creating opportunities for a meaningful day, and coaching towards employment goals. DSPs continue to be a part of the person's life, providing encouragement and emotional support during times of loss, grief, joy or excitement. Some DSPs are also assisting parents with disabilities to navigate parenthood. While providing supports and teaching life skills remains a priority for DSPs, facilitating, adapting, and accommodating life experiences similar to those of people without disabilities within the community has become core to achieving the outcomes people with IDD desire.
References
- Centers for Medicare and Medicaid Services (CMS). (2014). Medicaid program: State plan home and community-based services, 5-year period for waivers, provider payment reassignment, and home and community-based setting requirements for Community First Choice and Home and Community-Based Services (HCBS) waivers. 79 FR 2947.
personal story
“I Would Have Done That Forever and a Day”
Reflections of a Dad, and Former DSP

Robert with his youngest daughter, Morgan, who has an ASD diagnosis.
I am a Direct Support Professional (DSP). At least, I was. By the grace of the Almighty, I am also the happily married father of three spectacular, remarkable daughters, the youngest of which is an absolutely wonderful girl with autism spectrum disorder (ASD).
I started in the field of direct support at 18, back in 1995, working as support in a summer camp for adults with disabilities; I was paid $900 for the entire summer, as a one-time salary, which was considerably less than what I could make doing my usual summer landscaping. But it would afford me the opportunity to help make the lives of a few individuals with developmental disabilities better and more independent. During that summer I was hooked, and I kept coming back. All I needed to get started in the field was a clean driver’s license, my high school diploma, and showing up.
I spent my time on and off over many years within the field of direct support, occasionally leaving but always finding my way back, and watching it evolve. When I started working as a DSP, I was making — then — a decent starting wage of $8.00 an hour, with full health and dental. I was single at the time, didn’t have a family, and was still living at home, so it was entirely doable. Furthermore, I loved what I was doing because, where academia had failed somewhat to give me the ability to make a difference in the world, direct support honored me with the opportunity to transform others’ lives for the better. Because of the work I engaged in, someone who otherwise wouldn’t be able to experience independence, who wouldn’t be able to take part in our community, without whom our community would be greatly diminished, was a vibrant part of our community, a regular at the local coffee shop and video game store, and well known in his community. Though all of my training was on-the-job, through the direct mentoring of other DSPs I learned to engage in behavioral support, supporting activities of daily living, supporting independence, administering complex medications, and providing medically necessary routines and interventions. Left to myself, I would have done that forever and a day.
I REDOUBLED MY WORK IN DIRECT SUPPORT, AND DEVOTED MYSELF TO BUILDING THE PROFESSION INTO SOMETHING I COULD LEAVE MY DAUGHTER TO AND KNOW SHE WOULD BE CARED FOR AND SAFE.
Fast forward 20 years. I had three children, rent that had tripled, gas that had tripled in price, and I was still working in a field where the starting wage, on average, was $10 an hour, with bare-boned health and dental benefits, if any. I had just been promoted into frontline supervision and I was making, on average, slightly under $13 an hour, with work weeks that went 60+ hours. While I had earned my Master’s degree by this point, all I needed, as a professional qualification, was that high school diploma, a clean driving record, and continuing to show up.
We were living on my wife’s wages, and I was moonlighting as a tutor; many of my staff left my program each day to go work a second or third job, and often I became their ride to work because their wages were not such that they could afford to maintain their own vehicles. Each week, my wife and I had to make the decision whether I was going to keep doing DSP work, whether we could survive on the money coming into the house. What kept me going was my youngest daughter. She had been diagnosed with ASD, and between therapies, and the pressure of providing her all that she would need — an expense that is crippling to most families, let alone a family trying to live on a DSP’s salary — my wife and I were living the reality of ASD parents with all of the motivators and pressures that go with that. When you have a child with a disability, once you get over the shock of the diagnosis itself, you realize one of three things is true: Either you must become immortal, or you must outlive your child, or you must find someone to replace you when the time comes who will do justice to your child in the way you would. My bid for immortality wasn’t going so well, and no parent should ever have to outlive their child, so, my options were fairly clear. I redoubled my work in direct support, and devoted myself to building the profession into something I could leave my daughter to and know she would be cared for and safe.

At some point, we have to acknowledge that we are caring for, and providing for, the weakest and most vulnerable of our society through abusing the good will of DSPs who work two and three jobs; who must have public assistance to feed their families and stay within the field; and who willingly work holidays, weekends, and 16-hour double shifts just to see those individuals they support be a part of their communities. In so doing we are abusing those individuals that we, as a society, have an obligation to provide for and protect, individuals receiving direct support services.
At some point, we have to do better.
None of this should be taken as critique of provider agencies, supervisors or even executive teams that do what they can for Direct Support Professionals. Supervisors and administrators who make certain this doesn't happen on their watch should be strongly commended; they work tirelessly, without adequate, or even minimal, resources, but they can’t change the formulas that go into deciding rates paid for these services under Medicaid and Medicare. This does not change, however, the state of the system as a whole and the necessity of pointing out this glaring flaw. If that is negative, maybe a long, hard look at the system that could breed such negativity is called for.
Lastly, I say this not only as a former DSP (I’m now employed as a mental health counselor), but also as the father of a beautiful daughter with autism. I want her Direct Support Professionals to be well-trained, preferably degreed, and able to put their full attention on their work without having to hold second and third jobs or live below the poverty line to support her. This is a matter of protecting and respecting DSPs and those they support.
overview
Racial and Gender Disparities Within the Direct Support Workforce:
Five Key Findings
Despite their critical role in supporting older adults and people with disabilities nationwide, women in the direct support workforce — and women of color, in particular — are more likely than men to live in poverty. Women of color in direct support also have smaller family incomes and are more reliant on public benefits than their White counterparts. This article examines racial and gender disparities in the direct support workforce, with a focus on populations that have historically experienced differential treatment in employment. Specifically, we ask: How has the racial and gender composition of this workforce changed over the past 10 years, and how do race and gender shape the demographic, employment, and economic characteristics of the direct support workforce?
Snapshot of the Direct Support Workforce
The direct support workforce includes 4.5 million personal care aides, home health aides, and nursing assistants (PHI, 2017). They are largely employed in private homes, group homes, residential care facilities, assisted living residences, continuing care retirement facilities, nursing homes, and hospitals. In this article, direct support workers who work in private homes and community-based settings are referred to as "home care workers," while those who work in nursing homes are referred to as "nursing assistants." Direct support workers assist older adults and people living with disabilities with daily tasks, such as dressing, bathing, and eating. Personal care aides also help their clients with housekeeping and may assist them with errands, appointments, and social engagements outside of the home. Home health aides and nursing assistants perform some clinical tasks, such as blood pressure readings and assistance with range-of-motion exercises.
| ALL DIRECT SUPPORT WORKERS | HOME CARE WORKERS | NURSING ASSISTANTS | |||||
|---|---|---|---|---|---|---|---|
| GENDER | RACE/ETHNICITY | 2005 | 2015 | 2005 | 2015 | 2005 | 2015 |
| WOMEN | White | 44% | 39% | 41% | 36% | 45% | 42% |
| All People of Color | 45% | 48% | 50% | 51% | 46% | 49% | |
| Black or African American | 28% | 26% | 26% | 25% | 33% | 33% | |
| Hispanic or Latino (Any Race) | 11% | 14% | 18% | 19% | 7% | 10% | |
| Asian or Pacific Islander | 4% | 5% | 4% | 5% | 3% | 4% | |
| Other | 2% | 2% | 3% | 3% | 2% | 2% | |
| Total | 89% | 86% | 91% | 88% | 91% | 91% | |
| MEN | White | 6% | 6% | 4% | 5% | 4% | 4% |
| All People of Color | 6% | 8% | 4% | 7% | 5% | 5% | |
| Black or African American | 3% | 4% | 2% | 3% | 3% | 3% | |
| Hispanic or Latino (Any Race) | 1% | 2% | 1% | 2% | 1% | 1% | |
| Asian or Pacific Islander | 1% | 1% | 1% | 1% | 1% | 1% | |
| Other | 0% | 0% | 0% | 0% | 0% | 0% | |
| Total | 11% | 14% | 9% | 12% | 9% | 9% | |
| TOTAL | White | 50% | 45% | 45% | 42% | 50% | 46% |
| All People of Color | 50% | 55% | 55% | 58% | 50% | 54% | |
| Black or African American | 31% | 30% | 28% | 28% | 35% | 36% | |
| Hispanic or Latino (Any Race) | 13% | 16% | 19% | 21% | 8% | 11% | |
| Asian or Pacific Islander | 4% | 6% | 5% | 6% | 4% | 5% | |
| Other | 3% | 3% | 3% | 3% | 3% | 3% | |
| Total | 100% | 100% | 100% | 100% | 100% | 100% | |
5 Key Findings
To produce this statistical portrait of the racial and gender composition and disparities in the direct support workforce, we analyzed American Community Survey (ACS) data from 2005 to 2015 (see Tables 1-4). Race and ethnicity labels are mutually exclusive: "White," "Black or African American," "Asian or Pacific Islander," and "Other" do not include people who identify as "Hispanic or Latino." The "Other" category includes people who are American Indian, Alaska Native, two or more races, or some other race. We define "People of Color" as people who identify as a race other than White. We applied percentages from the ACS to Occupational Employment Statistics data compiled by the Bureau of Labor Statistics (BLS) to estimate the number of direct support workers in each gender and racial/ethnic cohort.
Using this methodology, we arrived at the following five key findings regarding racial and gender composition and disparities in the direct support workforce:
1. Women of color and men of all races are large and growing segments of the direct support workforce.
- From 2005 to 2015, women of color in direct support grew from 45% of the workforce (1.2 million workers) to 48% (1.7 million workers). Over the same period, men grew from 11% of the workforce (310,000 workers) to 14% (489,000 workers) (see Table 1).
- While the number of men who are nursing assistants remained the same during that period, the number of male home care workers tripled, growing from 60,000 in 2005 to 182,000 in 2015.
- Hispanic/Latina women in this workforce tend to work in home care and Black/African American women tend to work as nursing assistants. One in four home care workers (19%) is a Hispanic/Latina woman, compared to one in 10 nursing assistants (10%). One in three nursing assistants is a Black/African American woman (33%), compared to one in four home care workers (25%) (see Table 1).
2. Women in direct support tend to be older than men, regardless of race/ethnicity, and Asian/Pacific Islander direct support workers of all genders are older than their peers.
- The median age for women in the direct support workforce is 42 years old versus 37 years old for men (see Table 2).
- While direct support workers have similar median ages across most racial/ethnic groups, Asians and Pacific Islanders are the exception. The median age for Asian/Pacific Islander direct support workers is 48 years old — seven years older than the median age for all direct support workers.
| WOMEN OF COLOR | WHITE WOMEN | MEN OF COLOR | WHITE MEN | ALL WORKERS | |
|---|---|---|---|---|---|
| AGE | |||||
| 16-24 | 11% | 20% | 18% | 22% | 16% |
| 25-34 | 22% | 20% | 27% | 24% | 22% |
| 35-45 | 21% | 15% | 17% | 15% | 18% |
| 45-54 | 23% | 19% | 19% | 15% | 21% |
| 55-64 | 17% | 17% | 14% | 16% | 17% |
| 65+ | 6% | 8% | 5% | 8% | 7% |
| Median | 42 | 41 | 37 | 37 | 41 |
| EDUCATIONAL ATTAINMENT | |||||
| Less than High School | 19% | 9% | 11% | 9% | 14% |
| High School Graduate | 35% | 36% | 32% | 28% | 34% |
| Some College, No Degree | 30% | 36% | 33% | 33% | 33% |
| Associate's Degree or Higher | 16% | 20% | 24% | 30% | 19% |
| EMPLOYMENT STATUS | |||||
| Part-time or part-year | 59% | 65% | 49% | 57% | 60% |
| Full-time or full-year | 41% | 35% | 51% | 43% | 40% |
| EARNINGS AND INCOME | |||||
| Median Personal Earnings | $17,300 | $16,000 | $20,000 | $17,500 | $17,000 |
| Median Family Income | $43,400 | $52,900 | $56,300 | $60,800 | $49,100 |
| POVERTY LEVEL | |||||
| Less than 100% | 22% | 17% | 12% | 14% | 19% |
| Less than 138% | 34% | 27% | 22% | 22% | 30% |
| Less than 200% | 54% | 44% | 40% | 38% | 48% |
| PUBLIC ASSISTANCE | |||||
| Any Public Assistance | 49% | 39% | 34% | 35% | 43% |
| Food and Nutrition Assistance | 33% | 22% | 20% | 17% | 27% |
| Medicaid | 29% | 22% | 17% | 17% | 25% |
| Cash Assistance | 3% | 3% | 1% | 2% | 3% |
| HEALTH INSURANCE STATUS | |||||
| Any Health Insurance | 83% | 87% | 82% | 87% | 85% |
| Health Insurance Through Employer/Union | 43% | 53% | 54% | 55% | 48% |
| Medicaid, Medicare, or Other Public Coverage | 34% | 30% | 23% | 27% | 31% |
| Health Insurance Purchased Directly | 12% | 13% | 10% | 14% | 12% |
3. Women in direct support generally have lower levels of formal education than men, and White direct support workers generally have higher levels of formal education than direct support workers of color.
- Fifty-three percent of women of color and 45% of White women in the direct support workforce have a high school education or less, compared to 43% of men of color and 37% of White men (see Table 2).
- Women of color in direct support are twice as likely as their White counterparts to have less than a high school education. Nineteen percent of women of color in direct support have less than a high school education, compared to 9% of White women (see Table 2).
- Among Asian/Pacific Islander direct support workers, 69% of men and 57% of women have some college education or a college degree. However, many Asian/Pacific Islander workers have less than a high school education, including 20% of women and 12% of men. These findings suggest that educational attainment varies considerably within the highly diverse Asian/Pacific Islander population.
4. Women of color are more likely to live in poverty and rely on public assistance than their counterparts in the direct support workforce.
- The poverty rate for women of color in direct support (22%) is higher than the poverty rate for White women (17%), White men (14 %), and men of color (12%) (see Table 2).
- Forty-nine percent of women of color in direct support rely on public assistance, compared to 39% of White women, 35% of White men, and 34% of men of color in this workforce (see Table 2).
- People of color in direct support are generally more likely than White workers to live in poverty, though Asian/Pacific Islander direct support workers are an exception. Among Asian/Pacific Islander workers, 12% of women and 9% of men live in poverty, and 37% of women and 29% of men rely on public assistance.
5. Men and people of color in direct support have higher personal earnings than women and White workers, but White workers have higher family incomes than people of color.
- Men in direct support have higher personal earnings than women, while people of color in direct support have higher annual personal earnings than White workers. Median personal earnings are $20,000 for men of color and $17,500 for White men, whereas median personal earnings for women of color are $17,300, compared to $16,000 for White women (see Table 2).
- Annual earnings are an expression of hourly wages, hours worked, and weeks worked. While hourly wages are not captured by the American Community Survey, 41% of women of color and 35% of White women work full-time hours year-round, compared to 51% of men of color and 43% of White men (see Table 2).
- The median family income for women of color is $43,400, compared to $52,900 for White women, $56,300 for men of color, and $60,800 for White men (see Table 2).
- Asian/Pacific Islander direct support workers have higher personal and family incomes than other racial/ethnic groups — they typically earn $19,200 annually, and their families typically earn $68,300. However, there is more variation in earnings among Asian and Pacific Islander subgroups than within other racial/ethnic groups.
| WOMEN OF COLOR | WHITE WOMEN | MEN OF COLOR | WHITE MEN | ALL WORKERS | |
|---|---|---|---|---|---|
| AGE | |||||
| 16-24 | 8% | 12% | 15% | 17% | 11% |
| 25-34 | 19% | 17% | 26% | 22% | 19% |
| 35-45 | 20% | 16% | 17% | 13% | 18% |
| 45-54 | 25% | 24% | 19% | 20% | 24% |
| 55-64 | 20% | 20% | 17% | 17% | 20% |
| 65+ | 7% | 11% | 6% | 11% | 9% |
| Median | 45 | 47 | 39 | 43 | 45 |
| EDUCATIONAL ATTAINMENT | |||||
| Less than High School | 25% | 11% | 17% | 9% | 18% |
| High School Graduate | 34% | 36% | 34% | 29% | 35% |
| Some College, No Degree | 26% | 32% | 28% | 35% | 29% |
| Associate's Degree or Higher | 14% | 21% | 22% | 26% | 18% |
| EMPLOYMENT STATUS | |||||
| Part-time or part-year | 68% | 70% | 59% | 62% | 68% |
| Full-time or full-year | 32% | 30% | 41% | 38% | 32% |
| EARNINGS AND INCOME | |||||
| Median Personal Earnings | $14,000 | $13,000 | $15,800 | $15,000 | $13,800 |
| Median Family Income | $39,000 | $50,100 | $48,300 | $52,500 | $44,100 |
| POVERTY LEVEL | |||||
| Less than 100% | 27% | 19% | 16% | 16% | 23% |
| Less than 138% | 39% | 30% | 28% | 26% | 34% |
| Less than 200% | 59% | 46% | 47% | 44% | 53% |
| PUBLIC ASSISTANCE | |||||
| Any Public Assistance | 57% | 48% | 46% | 45% | 52% |
| Food and Nutrition Assistance | 38% | 26% | 26% | 23% | 32% |
| Medicaid | 35% | 26% | 25% | 21% | 31% |
| Cash Assistance | 4% | 3% | 1% | 4% | 3% |
| HEALTH INSURANCE STATUS | |||||
| Any Health Insurance | 80% | 85% | 79% | 82% | 82% |
| Health Insurance Through Employer/Union | 32% | 42% | 41% | 43% | 37% |
| Medicaid, Medicare, or Other Public Coverage | 42% | 38% | 33% | 33% | 40% |
| Health Insurance Purchased Directly | 12% | 16% | 11% | 15% | 13% |
| WOMEN OF COLOR | WHITE WOMEN | MEN OF COLOR | WHITE MEN | ALL WORKERS | |
|---|---|---|---|---|---|
| AGE | |||||
| 16-24 | 15% | 28% | 20% | 33% | 22% |
| 25-34 | 25% | 25% | 27% | 26% | 25% |
| 35-45 | 22% | 15% | 20% | 21% | 19% |
| 45-54 | 20% | 15% | 19% | 9% | 18% |
| 55-64 | 14% | 13% | 12% | 7% | 13% |
| 65+ | 3% | 3% | 3% | 5% | 3% |
| Median | 38 | 33 | 36 | 32 | 36 |
| EDUCATIONAL ATTAINMENT | |||||
| Less than High School | 13% | 10% | 8% | 15% | 12% |
| High School Graduate | 39% | 39% | 36% | 32% | 39% |
| Some College, No Degree | 34% | 38% | 34% | 29% | 36% |
| Associate's Degree or Higher | 14% | 12% | 22% | 24% | 14% |
| EMPLOYMENT STATUS | |||||
| Part-time or part-year | 50% | 59% | 38% | 51% | 53% |
| Full-time or full-year | 50% | 41% | 62% | 49% | 47% |
| EARNINGS AND INCOME | |||||
| Median Personal Earnings | $20,000 | $19,000 | $22,900 | $18,500 | $20,000 |
| Median Family Income | $44,100 | $51,100 | $61,100 | $58,700 | $48,000 |
| POVERTY LEVEL | |||||
| Less than 100% | 18% | 16% | 10% | 16% | 17% |
| Less than 138% | 32% | 26% | 16% | 26% | 29% |
| Less than 200% | 52% | 44% | 35% | 48% | 48% |
| PUBLIC ASSISTANCE | |||||
| Any Public Assistance | 46% | 34% | 26% | 32% | 39% |
| Food and Nutrition Assistance | 32% | 22% | 17% | 19% | 27% |
| Medicaid | 26% | 20% | 11% | 15% | 22% |
| Cash Assistance | 2% | 3% | 1% | 1% | 2% |
| HEALTH INSURANCE STATUS | |||||
| Any Health Insurance | 85% | 88% | 83% | 87% | 86% |
| Health Insurance Through Employer/Union | 51% | 61% | 64% | 62% | 56% |
| Medicaid, Medicare, or Other Public Coverage | 29% | 23% | 15% | 19% | 26% |
| Health Insurance Purchased Directly | 11% | 10% | 8% | 11% | 11% |
Conclusion
In the coming decades, millions of older adults and people with disabilities will increasingly rely on direct support workers for assistance, and women of color will be critical to meeting this demand. Women of color make up the largest and fastest-growing segment of the direct support workforce — from 2005 to 2015, the number of women of color in direct support grew from 1.2 million to 1.7 million. In addition, from 2016 to 2026, the number of women of color in the labor force is projected to grow by 6.3 million workers, while the number of White women in the labor force is projected to decline by 384,000 over the same time period (U.S. Bureau of Labor Statistics, 2015).
Unfortunately, direct support jobs do not provide economic stability to women of color and their families — they are generally more likely to live in poverty and rely on public benefits than their counterparts, and they have smaller family incomes to rely on for support. In this context, improving the economic well-being of women of color in direct support would improve their quality of life, and it would help attract workers to this important occupation, as well as help retain them. More research is needed on the many diverse populations described in this article, particularly in regard to improving their economic stability.
Additionally, while women constitute the largest segment of the direct support workforce, men are increasingly joining their ranks — the number of men in direct care grew from 310,000 in 2005 to 489,000 in 2015. This research also shows that the characteristics of men in direct support are distinct from those of women in several respects: they are younger, more educated, and live in higher-income households than women in the profession. Further research would help explain these differences, as well as identify strategies to recruit more men into the direct support workforce.
References
- PHI (2017, Nov. 10). Workforce data center.
- U.S. Bureau of Labor Statistics (BLS), Employment Projections Program (2015). Employment projections: 2016—2026, Table 3.4 Civilian labor force by age, sex, race, and ethnicity, 1996, 2006, 2016, and projected 2026 (Numbers in thousands). Analysis by PHI (October 25, 2017).
overview
Learn, Lead, Love:
The Journey Toward Excellence in Direct Support
The approach to supporting people with intellectual and/or developmental disabilities has shifted over the past several years as more and more people live outside of institutions in community residences and in their own homes. The change has transformed the way we think about staff support from "taking care" of individuals to "working with" and supporting individuals to live in inclusive communities. These changes have also required that the workforce understand emerging concepts such as inclusion, self-advocacy, person-centered planning, positive behavior support, supported living and employment, supported decision-making, and much more.
For many years, however, this new language of community support skills, knowledge, and ethics was not organized in a coherent and accessible manner useful to trainers and educators. This meant that direct support staff did not receive systematic instruction in community-based support strategies and were poorly equipped to provide the kind of support that helped people achieve their dreams of full community participation. Nor were direct support staff recognized as professionals performing complex and nuanced skills, which left this workforce undervalued and underpaid. This began to change in 1993 when the federal government recognized the importance of strengthening many occupations essential to the American workforce, and provided resources to identify the skills and knowledge needed by entry-level workers in a range of occupations.
The First Step: Learn
The human services field was one of 22 American industries that received funding in 1993 to create a nationally-developed and validated professional core of knowledge and skills. Human Services Research Institute (HSRI) — an organization providing research, support, and guidance to clients nationwide looking to develop more efficient and responsive service systems — undertook this work in collaboration with the Educational Development Center — a non-profit collaborating with public and private partners to create, deliver, and evaluate programs, services, and products. Together with a coalition of stakeholders from across the country that included college and high school level educators, human services employers, advocates and self-advocates, families and other key partners, the project staff and its stakeholder advisors worked collaboratively over a three-year period to convene hundreds of Direct Support Professionals (DSPs) across the country serving a diverse group of participants, all of whom relied on long-term support.
The groups included people with intellectual and/or developmental disabilities, older people with support needs, people with psychiatric challenges, and people with physical disabilities. Using the gold standard process for identifying core skills and knowledge called "Developing a Curriculum" or DACUM, the project team worked with these groups of direct support staff to build consensus on the core skills, knowledge sets, and work performance indicators most important to help people live full and satisfying lives. After an extensive national validation process these Community Support Skill Standards (CSSS) were published and widely disseminated, with the goal of helping DSPs learn the most updated and valid skills and knowledge essential to quality community support (Taylor, Bradley, & Warren, 1996).
Many professions, especially those that require relationships of trust with their clients, weave together the two strands of core skills and knowledge with an essential third strand of "ethics" to guide the workers’ choices, commitment, and behavior in performing their jobs. This critical third element was added as a corollary to the Skill Standards in 2001 when the President’s Committee on Persons with Intellectual Disabilities (formerly PCMR) provided support for a stakeholder advisory group to develop and validate ethical guidelines. This meant that in addition to the knowledge and skill at the core of the profession, direct support staff were also able to learn important values-based practices that assured a respectful and ethical posture in their work (see Figure 1).
The Code of Ethics developed through the National Alliance for Direct Support Professionals (NADSP) guides DSPs through the ethical dilemmas they face daily and encourages the highest professional ideals. Direct support staff, agency leaders, policymakers, and people receiving services are urged to read the code and to consider ways that these ethical statements can be incorporated into daily practice. This code is not the handbook of the profession, but rather a roadmap to assist in staying the course of securing freedom, justice, and equality for all.
- Person-Centered Supports. As a DSP, my first allegiance is to the person I support; all other activities and functions I perform flow from this allegiance.
- Promoting Physical and Emotional Well-Being. As a DSP, I am responsible for supporting the emotional, physical, and personal well-being of the individuals receiving support. I will encourage growth and recognize the autonomy of the individuals receiving support while being attentive and energetic in reducing their risk of harm.
- Integrity and Responsibility. As a DSP, I will support the mission and vitality of my profession to assist people in leading self-directed lives and to foster a spirit of partnership with the people I support, other professionals, and the community.
- Confidentiality. As a DSP, I will safeguard and respect the confidentiality and privacy of the people I support.
- Justice, Fairness and Equity. As a DSP, I will promote and practice justice, fairness, and equity for the people I support and the community as a whole. I will affirm the human rights, civil rights and responsibilities of the people I support.
- Respect. As a DSP, I will respect the human dignity and uniqueness of the people I support. I will recognize each person I support as valuable and help others understand their value.
- Relationships. As a DSP, I will assist the people I support to develop and maintain relationships.
- Self-Determination. As a DSP, I will assist the people I support to direct the course of their own lives.
- Advocacy. As a DSP, I will advocate with the people I support for justice, inclusion, and full community participation.
Next Step: Lead
As the institutional wall began to come down, a new language of community living was created and many tools, including the CSSS, were created to help support individuals to life fulfilling community lives. But, where did the CSSS lead?
First, the collaborative aspects of the CSSS project, including its diverse national stakeholder group and the many other stakeholders and direct support staff gathered under the project’s DACUM umbrella, forged personal and professional connections that have sustained and grown over decades. These provided leadership in the development of the direct support workforce. One enduring outcome of the CSSS and other leadership efforts was the establishment of the National Alliance for Direct Support Professionals (NADSP;). The University of Minnesota’s Research and Training Center on Community Living and HSRI offered substantial guidance and support in the creation of the Alliance. Through the adoption of the term "Direct Support Professional" in its title and in the many projects and publications generated by members of NADSP, this term has been adopted nationally to signify a person performing direct support who is competent, knowledgeable, and ethical. Further, NADSP has developed a multi-level, national, voluntary certificate program based on the CSSS through which direct support staff across the country who meet its requirements may obtain this rigorous certificate status. In addition to providing a certification program, NADSP is active in advocating for better wages and work conditions, building partnerships with self-advocates and human service professional organizations, and providing high quality training for DSPs.
Another group with a substantial focus on direct support — the Mid-Hudson Coalition, a group of human services employers in New York State — has made good use of the CSSS by reaching out to local community colleges to communicate the skills and knowledge sets most desired in their workforce. Both community colleges serving this region, SUNY Ulster and Duchess Community College, have developed certificate programs aligned with the standards.
In Massachusetts, the state’s Department of Developmental Services (DDS) worked with community colleges to create a certificate program aligned with the CSSS. The tuition is paid by the Massachusetts DDS in partnership with employers whose DSPs attend the certificate program. Bristol Community College in Massachusetts used the standards to create a core track of coursework to prepare students to enter either human services or health care degree program.
Using the CSSS and other resources, Georgia offers a community college-based certificate that fully engages people with disabilities as "learning partners" to help DSPs master important skills and knowledge within the context of a respectful learning partnership. This program has been replicated in New Hampshire.
Perhaps the most widespread application of the CSSS has occurred within the online direct support educational program called the College of Direct Support, which is now part of a suite of online learning products called DirectCourse. The platform is supported by Elsevier (an educational publisher) with content development expertise from the University of Minnesota’s Research and Training Center on Community Living and a board of content editors. The College of Direct Support offers an array of online courses whose target audience is DSPs working with people with intellectual and developmental disabilities. The courses are carefully aligned with the CSSS and the code of ethics. Over 9 million learners have enrolled in the College of Direct support since it began, and have completed nearly 12.6 million lessons.
Another enduring application of the CSSS was initiated by the Ohio Chapter of NADSP and the state’s Developmental Disability Council, and resulted in the creation of an architecture for an employer sponsored certificate program based on the CSSS called Ohio DSPATHS. PATHS employs a unique skills mentoring role in the certificate that partners certified and skilled DSPs as skills mentors to DSP learners, providing both a career path and substantive support to learners. This project vastly increased the collaboration of individual employers across the state in joint efforts to strengthen the workforce. At certificate graduate events their work is celebrated, and selected work portfolios are read, offering inspiration and a window into the everyday accomplishments of DSPs.
Goal of the Journey: Love
Beyond the anchors of a profession — skills, knowledge and ethics — it is important to think about why people choose direct support. This is especially important when the economy is good and DSPs are hard to find. The work cannot be captured solely in a skills grid or listing of competencies. People who choose to do the work are motivated by both heart and spirit that engenders deep concern for the well-being of others. Some may not be fully aware of this when they come into the work, but become uplifted and often loved by the people they support. Many DSPs find enormous satisfaction and joy in this experience. Simply, it is one more opportunity to love and be loved. Relationship is a vector that carries love and learning in two directions and the direct support profession is all about relationship and support in community. As Parker J. Palmer wrote in Let Your Life Speak: "When we live in the close-knit ecosystem called community, everyone follows, and everyone leads" (Palmer, 1999, p. 74).
References
- Palmer, P. (1999). Let your life speak: Listening for the voice of vocation. San Francisco: Jossey-Bass.
- Taylor, M., Bradley, V., & Warren, R. Jr. (Eds.). (1996). The community support skill standards: Tools for managing change and achieving outcomes. Skill standards for direct service workers in the human services. Cambridge MA: HSRI.
overview
Why Competency-Based Credentialing for the Direct Support Workforce?
In college, I lived with a nursing student who completed a credential to work as a certified nursing assistant (CNA). For college work, she had an awesome gig. She was working alongside nurses, gaining important professional experiences, and she was paid decent wages. The credential she earned also meant something to her professionally; it was something she listed on her resume as she advanced in her career. At the same time, I worked as a personal care assistant, providing support for a young girl living in her family home. Some supports I provided were similar to those my roommate provided as a CNA: I attended to her medication and health needs. I also assisted with her physical endurance goals. I helped motivate her to get out of her wheelchair and learn to use her walker. We walked around her neighborhood as she strengthened her legs and arms. I assisted her with her schoolwork, and took her to the park to play with other children. This work was outstandingly meaningful to me, and it certainly shaped my professional interests. Unfortunately, I never considered this work as a career or a stepping stone on the pathway to my professional goals. My training for this position was minimal, and I never received specialized training for my role beyond viewing a preservice training video at the organization that sent me my paycheck. Following that, I never again stepped foot in the organization’s administrative building for the years that I worked with this child.
Later in my career I learned the term "Direct Support Professional," which encapsulates several job titles including personal care assistants. Direct Support Professionals (DSPs) play a vitally important role in supporting people with intellectual and developmental disabilities to live, work, and enjoy living in their communities. Given their close, consistent proximity to the people for whom they provide support, DSPs can support peoples’ self-determination, independence, and social participation. Well-trained DSPs will provide person-centered supports, and maximal opportunities for a person to exercise choice and participate in their community. As such, the role of the DSP is specialized, and contrasts with other support professions, such as CNAs. However, implementation of preservice and professional development training has not kept up with the demand for DSPs to provide high quality supports for people in the community. The aim of this article is to present a brief overview of professional development opportunities for the direct support workforce. A special emphasis is given to competency-based credentialing because of its potential to professionalize the important work performed by this high-demand workforce.
Professional Development in the Direct Support Workforce
State and federal regulations are largely silent about mandated preservice and in-service training for DSPs (Marquand, 2013). Some states that do require preservice training often focus on basic skills such as CPR, first aid, and documentation. There is often little focus on person-centered services or supporting a person’s self-determination. Even in states with a high standard for preservice and in-service training, organizations have a difficult time keeping up with the delivery of them. In 2015, the Research and Training Center on Community Living (RTC-CL) at the University of Minnesota, in conjunction with the New York State Association of Community and Residential Agencies (NYSACRA) and the New York State Rehabilitation Association (NYSRA), conducted a research study that included 206 provider organizations in New York state. New York requires 100 hours of preservice training, but organizations reported that DSPs received an average of 50 hours of preservice training, and 33 average hours of training in subsequent years (Hewitt, Taylor, Kramme, Pettingel & Sedlezky, 2015). The scant number of training hours delivered to DSPs can be compared to the minimum 75-hour preservice education requried to become a CNA or home health aide. Many difficulties can interfere with completion of DSP training. These include (a) federal reimbursement rates that cover little more than personnel costs; (b) the wide dispersal of DSPs across different work sites rather than the centralized location where training is provided; (c) difficulty finding time to deliver training due to the widely varying hours worked by DSPs; and (d) the high vacancy rate in DSP positions, which makes it difficult to cover shifts while DSPs attend training. Despite this, a series of focus groups conducted during this same study indicated that DSPs were anxious to learn more, develop their skills, and continue careers in the field.

- CSSS 1996: Community Support Skill Standards
- Hewitt 1998: IDD Residential Core
- NADSP 2002: National Alliance for Direct Support Professionals Core Competencies
- APSE 2011: Association of People Supporting Employment
- DOL LTSS 2012: Department of Labor Long-Term Services and Supports Core Competencies
- FLS 2013: National Frontline Supervisor Core Competencies
- NADD 2014: National Association of Dual Diagnosis Competency-Based Direct Support Certification
- CMS 2014: Centers for Medicare and Medicaid Services DSP Core Competencies
Competency-Based Training
Several direct support workforce competency sets have been identified and refined in response to recognizing and profesionalizing this unique and important workforce. Competency sets delineate the necessary knowledge, skills, and attitudes needed to provide high quality supports. Figure 1 depicts these national professional competency sets. These sets have been validated by an array of stakeholders, which included people receiving services, family members, guardians, DSPs, supervisors, and agency administrators. The competencies have evolved in response to the demands of increasingly individualized and self-directed services.
A widely used and recently updated set of competencies that specifically apply to DSPs was adopted by the National Alliance for Direct Support Professionals (NADSP). There are 15 competencies with corresponding skill statements characteristic of DSPs providing quality supports on the job. Figure 2 identifies these 15 core competencies for DSPs.
Many anecdotal reports indicate the increased quality of supports provided by DSPs whose professional development is aligned with these nationally validated core competencies. In addition, a large-scale randomized control trial of a training program aligned with the NADSP core competencies indicated a significant decrease in an organizations’ DSP turnover rates compared to organizations who did not implement the training (Bogenshutz, Nord, & Hewitt, 2015). This could indicate that DSPs felt more prepared for, satisfied with, and committed to their jobs. These competencies are the basis for credentialing programs offered by organizations across the nation.
The NADSP Competency Areas: The Foundation of the Work
- Area 1: Participant Empowerment
- Area 2: Communication
- Area 3: Assessment
- Area 4: Community and Service Networking
- Area 5: Facilitation of Services
- Area 6: Community Living Skills and Supports
- Area 7: Education, Training, and Self-Development
- Area 8: Advocacy
- Area 9: Vocational, Educational, and Career Support
- Area 10: Crisis Prevention and Intervention
- Area 11: Organizational Participation
- Area 12: Documentation
- Area 13: Building and Maintaining Friendships and Relationship
- Area 14: Person-Centered Supports
- Area 15: Supporting Health and Wellness
Implementing Credentialing and Career Ladder Opportunities
Competency-based credentialing opportunities for the direct support workforce are being implemented at some organizations across the U.S. In 2014, RTC-CL worked with the Office for People with Developmental Disabilities (OPWDD) in New York state to create recommendations for programmatic and financial implications of implementing a voluntary statewide workforce credentialing program. This project included many phases and was guided by an advisory committee that included people receiving supports, DSPs, supervisors, administrators, OPWDD personnel, and provider organizations in New York. This study included a literature review, environmental scan, a series of focus groups across the state, and a quantitative survey completed by provider organizations. From these data RTC-CL created succinct recommendations for implementing a successful statewide credentialing program, a financial model that delineated costs for the first five years of implementation, and a marketing plan for promoting it across the state. The recommendations called for a multi-tiered model that utilizes a variety of educational delivery methods, including on-the-job training to ensure that DSPs generalize the skills they learn in coursework. The multi-tiered model created for the state of New York is depicted in Figure 3. DSPs who completed the first credential could work on the second credential and so forth in order to continue specializing their skill set. Each credential tier was paired with an hourly wage increase commensurate to the amount of time associated with advancing their skills.
Advocacy efforts are still underway in New York to implement the credential model and receive legislative support. At the RTC-CL, staff are currently working with several organizational or cooperative workforce credentialing efforts in New York to summarize the ways they are utilizing credentialing, and how it has impacted the workforce. These organizations unanimously report that the supports provided by credentialed DSPs are of high quality. One example of a way that an organization is noticing this impact is by the involvement of its DSPs pursuing credentialing in individualized support planning meetings. Before participating in the credentialing program, none of the DSPs participated in these meetings. After participation, and with the permission of the individual they supported, all employees pursuing the credential at the organization determined that it was their place to attend these meetings. Participation in the credentialing program has helped the DSPs to better understand delivery of person-centered services and their role in supporting people to achieve the person’s plan.

- DSP Credential I: 50 Hours
- DSP Credential II: 100 Hours
- DSP Credential III (Mentor): 40 Hours
- Frontline Supervisor & Management: 40 Hours
Conclusion
Currently, implementation of certification or credentialing programs similar to CNA programs does not widely exist for DSPs. Organizations and states that are implementing or seeking to implement workforce credentialing programs do so for three primary reasons: Successful completion of a professional credential increases justification for raising wages and investment in highly skilled DSPs; credentialing programs help professionalize the field through a career pathway and occupational recognition; and well-designed credentialing programs provide targeted educational opportunities to learn new skills while working, increasing the quality of supports. As credentialing efforts across the nation gain momentum, they are promising in terms of their ability to stabilize the direct support workforce, provide professional development opportunities for DSPs, and ultimately improve quality of life of people with intellectual and developmental disabilities.
References
- Bogenschutz, M., Nord, D., & Hewitt, A. (2015). Competency-based training and worker turnover in community supports for people with IDD: Results from a group randomized controlled study. Intellectual and Developmental Disabilities, 53, 182-195. doi:10.1352/1934-9556-53.3.182
- Hewitt, A., Lakin, C., Macbeth, J. Kramme, J., & Benway, C. (2018). President’s committee for people with intellectual disabilities report to the president 2017: America’s direct support workforce crisis — Effects on people with intellectual disabilities, families, communities and the U.S. economy. Washington D.C.: President’s Committee for People with Intellectual Disabilities.
- Hewitt, A., Taylor, M., Kramme, J., Pettingell, S., & Sedlezky, L. (2015). Implementing direct support professional credentialing in New York: Technical report. Minneapolis: University of Minnesota, Institute on Community Integration, Research and Training Center on Community Living.
- Marquand, A. (2013). Personal care aide training: Summary of state findings. Bronx, NY: Paraprofessional Healthcare Institute.
- National Alliance for Direct Support Professionals (NADSP) (2018). 15 NADSP competency areas.
personal story
“We Have to Use Every Creative Idea We Have”:
An Agency Director Looks at the Direct Support Crisis

"I have big news about your nephew," my mother shared recently in our daily phone chat. "They have a place for him in a group home," she continued. In this case, "they" is a very good organization run by a friend of mine. The "group home" is a typical house he would share with three other guys in a regular neighborhood in southeast Iowa.
My nephew is a fun-loving person who is obsessed with his smart phone, loves to ride his wave runner, is a reliable employee, and also has an intellectual disability, an anxiety disorder, and obsessive compulsive disorder. After talking to him, I learned he is approaching this change with a "still under consideration" mindset. Everyone else is very excited. I, too, am excited, for this next chapter of his life to begin, for the friendships I know he’ll form, and for him to enjoy additional independence. But, my excitement is also mixed with a sense of apprehension.
My uneasiness is driven by an understanding that in our community services for people with intellectual and/or developmental disabilities (IDD) we are never any better than our Direct Support Professionals (DSPs). And, we are in the midst of a developing direct support workforce crisis — one that creates a serious problem for us and the people we serve. Turnover, recruitment, and retention have been bad for a long time, and in many places things are getting worse.
Direct Support Professionals do the real work in organizations that provide community services. They help people acquire needed skills to live successfully, get jobs, develop social networks, and explore interests that turn into activities that lead to true participation and inclusion. DSPs are often the cultural guides that help people with IDD navigate their communities and find their places in them.
Those are the obvious impacts of DSPs; there are many far more subtle. DSPs are a key confidante and advocate for those with whom they work; they develop trusting relationships, they nurture and support, and the most talented of them are able to work from a basis of kindness and compassion that multiplies their effectiveness. It’s a fine line we are asking DSPs to walk, yet I see staff do so successfully every day in our organization.
Like any responsible organization we have spent years working to improve our DSP recruitment and retention. We have substantially increased wages several times, and our benefit package is among the best in the industry. We have invested in training for our DSPs to make sure they have the skills to do their jobs. Believing front-line supervisors are key to this equation we have invested in their training and worked to equip them to provide great supervision and support to DSPs. Yet, our turnover ticks up.
LIKE ANY RESPONSIBLE ORGANIZATION WE HAVE SPENT YEARS WORKING TO IMPROVE OUR DSP RECRUITMENT AND RETENTION. YET, OUR TURNOVER TICKS UP.
Making all our efforts more challenging is the fact that as a predominantly Medicaid-funded service we have limited access to rate increases that would allow us make substantial changes in pay and benefits. The result continues to be DSPs holding vital and challenging jobs for which they are just not paid enough. Changing regulatory requirements now put pressure on organizations to produce Medicaid-compliant documentation; this causes DSPs to take precious time away from those they support to meet documentation expectations. In staff surveys, DSPs articulately tell us what frustrates them about their jobs — bureaucratic requirements, poor communication, not feeling like valued members of the service team, low pay. What keeps them in their jobs? Their commitment to the people they support. Loved ones of people we serve are blunt about the changing regulatory environment: "All they seem to do is sit behind their computers" is an often-heard concern.

We see the impacts of high turnover and recruitment challenges everywhere we look. Moms and dads of people we have supported for decades continue to worry about staff changes, fearing the next one will negatively impact their loved one. A missed medication, not understanding the nuances of communication, or simply not investing in their loved one — there is so much that can go wrong. Existing DSPs work far too many hours, and frontline supervisors and other managers fill in for open shifts. While not a bad thing occasionally, there are clear increases in stress and overall negative impacts on employee morale when this becomes a routine part of the staffing solution. And, with few other options, it has become a routine part of staffing in many organizations. Overworking existing DSPs and other supervisors as they fill in for vacant positions provides a paradoxical solution; the work is covered in the short run, but it leads to rapid burnout and exhaustion and often results in increased turnover.
So what do we do about all of this? This is a complex problem and we need to treat it as such. The work of DSPs is both challenging and demanding and it must pay a living wage. To that end our advocacy for adequate funding simply has to continue, even in this fiscally challenging environment. It is critical we leverage all support offered by technology so people with disabilities can live with more privacy while still having access to help when needed, and allowing us to deploy staff only when absolutely necessary. We have to use every creative idea we have to capture capable and interested people — and hang onto them — such as career ladders or lattices, early outreach to high school students, and meaningful internships.
Very nearly 35 years ago I got my start in the field of disability services as a houseparent. My wife and I worked together and it was a wonderful job, one that continues to shape our perspective and career choices. I believe DSPs provide critical services. But, everything hangs in the balance for my nephew and other people with IDD needing supports. For people with disabilities to live in and become a true member of their communities, we have to have an adequate supply of well-trained DSPs. Let’s work together to prospect for solutions to this thorny problem. History will judge us on how well we navigate this moment.
overview
Workplace Culture Drives or Drags DSP Performance
If you ask savvy directors of agencies serving persons with intellectual and other developmental disabilities (IDD) to name their most important resource without which there would be no mission, they will not say "money." Direct Support Professionals (DSPs) are the principal resource, and funding, though important, is secondary.
DSPs represent 80% of an agency’s workforce and are functionally responsible for most day-to-day quality supports needed by persons with IDD. They are scarcer than ever for reasons that are all too obvious — turnover rates, demographic shifts, occupational non-recognition, and compensation. Remedies seem out of reach. Experience and common wisdom reveal that stabilizing the DSP workforce begins with concerted retention efforts. Workplace culture development is both a retention commitment and a quality enhancer, requiring little money yet serious effort (see Figure 1).
CULTURE IS ONLY AS GOOD AS THE PEOPLE DECIDE IT SHOULD BE. CULTURE IS THE MEDIUM WHICH HOLDS THE MISSION IN ITS HANDS AND DETERMINES ITS SUCCESS.
What is Workplace Culture?
Culture is the personality of an organization, an amalgam of collective memories and experiences that generate written and unwritten rules. Culture is what it feels like to work for a specific employer.
Culture is the silent given. It precedes and surrounds all employees, and it is defined either by what is allowed or what is deliberately created. Culture is the medium in which people work. Mission, strategy, and outcomes are all accomplished by people, and people are deeply affected by their culture. How DSPs are affected in their work is the manifestation of their culture. Further, all culture is local; namely, the culture or subculture in which DSPs spend the most time wields the strongest influence over them.
Metaphorically, culture in our workplace is the air we breathe (e.g., fresh, foul, invigorating or stale); the climate in which we function (e.g., hot, cold, unpredictable); and its members’ brand or style (e.g., friendly, unfriendly, supportive, role-oriented, achievement-based, competitive, power-wielding). Culture will define the health and productivity of the organization in ways that sustain or poison. In this sense, culture is contagious and is everyone’s responsibility.
Culture is only as good as the people decide it should be. Culture is the medium which holds the mission in its hands and determines its success. In order to engender mission loyalty and personal ownership of responsibilities, every segment of the workplace must be a part of its improvement. The quality of DSP work depends on its culture, a culture that will either drive or drag it.
Workplace culture is complicated, but it is not mysterious. It is a human enterprise that organizes itself both deliberately and silently, breeding certain characteristics into the organization’s DNA. These markers are real and some have a kudzu-like root system; however, markers are not so rooted that they cannot be removed and replaced. For example, it is difficult but not impossible in a large organization to bend incrementally its vertical, author-itarian leadership to a more horizontal interpersonal, people-friendly approach.

Workplace Culture is More thant Morale
Improving workplace culture is not simply about feeling supported or coddled; work can be difficult and uncomfortable. Notably, culture is not morale, but rather morale is the prevailing temperament or symptom of a culture. One cannot cheer-up a culture by trying to boost its disposition. The process requires open-minded leadership that unearths staff perceptions and assumptions while remaining unthreatened by the responses and demonstrating the courage to make changes. For example, a leader may assemble a focus group and assign the task of giving words to the unwritten rules that exist beneath the surface in all workplace cultures: getting along, getting ahead, getting by, getting in trouble, getting out of trouble. They may inquire further about what else is allowed silently that deserves to be spoken aloud and given a chance to change. Some responses may be discomfiting. It is impossible for leaders to learn what they think they already know.
Examples of Positive Steps for Culture Improvement
Initiatives, tools, and exercises for assessing and improving workplace culture may be accessed through a range of sources, including:
- Realistic job preview protocols
- Staff development resources from organizations such as the National Alliance for Direct Support Professionals
- National accreditations that set high industry-performance standards, such as that from the Council on Quality and Leadership
- Broad use of National Core Indicators surveys
- Adoption of performance evaluations that include the practice of a code of ethics and set of validated core competencies
- Published tools that help to diagnose an existing organizational culture
- 360-degree evaluations for all staff
- Inventories that assess leadership performance in comparison with other leaders
- DSP organizational participation in information-sharing and decision-making
- Listening tours that inform strategy
- Simple human recognition of and regular interaction with DSPs
- Remunerated peer skill-mentorship programs
- DSP welcoming protocols
- Learn-and-earn incentives
- Frontline supervisor development
Frontline supervisor skills remain key to the retention of DSPs because supervisors interpret organizational culture to the DSP workforce. Administration and middle management must exhibit a cascading commitment to excellence and capacity building, but the most powerful focus within an organization remains the frontline supervisor and their skills in identifying effective process and tracking outcomes, interrelationship skills, coaching techniques, teamwork, self-awareness, and innovation.
Conclusion
If the nobility of human services is a commitment to honor the disability among those served and enable abilities to grow to their potential, the portrait of a desirable culture is one of ongoing development, self-determination, responsiveness, and positive relationships. People want to feel a part of such an organization, enjoy a team spirit, and experience the blending of personal values consistent with those of the organization. In this context, DSPs and other employees of the organization achieve and exceed quality metrics because they have the staying power, will, and encouragement to do so. Commitment to intrinsic excellence is a powerful game-changer compared with external standards compliance and task mastering.
A workplace that decides its service culture and financial success rest on personal outcomes for people with IDD will experience a concomitant shift in the locus of power from executive to person-supported. In this sense, the person with IDD becomes the most important person in the system. Logically and strategically, the second-most important person is the DSP.
program profile
Proof of Professionalism:
NADSP Certification Programs
Since 2007, the National Alliance for Direct Support Professionals (NADSP) has offered a voluntary, national certification program for Direct Support Professionals (DSPs) working in community human service settings. The purpose of NADSP certification is to provide national recognition for DSPs who are delivering support consistent with the national standards established by NADSP’s Code of Ethics and 15 competency areas for DSPs.
Both the outcome of achieving national certification and the process itself can be valuable for DSPs, their employers, and the people they support. The applicants themselves acquire the knowledge, skills, and values needed to be more effective and more independent on the job. Employers of certified DSPs can proudly market their employment of nationally certified staff to potential clients, and provide greater assurances of quality to policymakers and funders. People supported by certified DSPs can partner with true professionals whose support is consistent with NADSP’s national standards.

The First NADSP Certification Framework
At its launch in 2007, the NADSP Certification Program for Direct Support Professionals (called NADSP Credentialing at the time) was made up of three levels: DSP-Registered, DSP-Certified, and DSP-Specialist:
- DSP-Registered (DSP-R). The entry-level credential for DSPs that allows them to show their intention to pursue a career in community human services. DSP-R requires being an employee in good standing with at least six months experience, a signed commitment to the NADSP Code of Ethics, and a statement of professional commitment from the DSP. Since inception, 9,705 DSPs have become DSP-Registered.
- DSP-Certified (DSP-C). Recognizes DSPs whose work has reached a level of competence consistent with NADSP standards. This level required the submission of a professional portfolio containing work samples tied to 8 of the 15 NADSP Competency Areas for DSPs. In addition to these work samples, the portfolio included documentation of the completion of 200 hours of NADSP-accredited education.
- DSP-Specialist (DSP-S). Recognizes certified DSPs who wanted to pursue specialization in any of the following specialty areas: Inclusion, Health Support, Employment Support, Mentoring and Supervision, Positive Behavior Support, or Aging. Applying for DSP-Specialist involved submitting a portfolio containing three work samples tied to the specialty area and 40 hours of employer-approved continuing education related to the specialty.
Today's NADSP Certification
Changes have been made in the NADSP certification program over the years, always with the intention of making the process more user-friendly for the applicants. They include:
- NADSP Certified-Initial (DSP-I) and NADSP Certified-Advanced (DSP-II). In 2013, the original DSP-Certified level was split into NADSP Certified-Initial (DSP-I) and NADSP Certified-Advanced (DSP-II), with each level requiring four work samples and 100 hours of NADSP-accredited education. Since 2007, 350 DSPs have achieved either DSP-I, DSP-II or the original DSP-C Certification.
- NADSP-Certified Specialist (DSP-III). The Specialist level was renamed NADSP-Certified Specialist (DSP-III), and the specialty in Mentoring and Supervision was later replaced with a stand-alone certification for frontline supervisors of DSPs.
- NADSP Frontline Supervisor Certification (FLS). Launched in 2014, it requires the submission of three work samples tied to 3 of the 11 National Frontline Supervisor Competencies, as well as 50 hours of NADSP-accredited education for frontline supervisors. One DSP has achieved the DSP-III certification, while 10 frontline supervisors have been awarded the FLS certification.
NADSP certification focuses on the practical application of an applicant’s knowledge, skills, and values on the job. Rather than focusing merely on what an applicant knows, the portfolio process instead focuses on the applicant’s work. Applicants have reported finding the portfolio development process to be a valuable experience. This emphasis on application also often results in positive outcomes for the people that the applicant supports. People being supported by DSPs seeking certification have gotten jobs, reunited with family members, and achieved positive health outcomes as a result of work that DSPs have included in their portfolios.
Coming Next: NADSP E-Badge Academy
Some DSPs have reported finding portfolio development to be overwhelming, especially when first starting the process. Another challenge is that the applicant does not receive any feedback from NADSP until after their portfolio is completed and submitted. This meant that misunderstandings about NADSP’s requirements might persist throughout the portfolio-construction period, sometimes for over a year. This feedback from DSPs led to NADSP efforts to develop an alternative to its traditional certification program.

At its 2017 national conference, NADSP announced the creation of the E-Badge Academy, to be launched in 2018. The electronic badges that make up the E-Badge Academy can be earned for completing hours of NADSP accredited education, committing to the NADSP Code of Ethics, and describing specific work by the applicant which is consistent with particular NADSP competencies.
Rather than submitting an entire portfolio containing multiple work samples, participants in the E-Badge Academy apply for each badge individually. In most cases the applicant applies for a badge by submitting a testimonial describing completed work that meets the requirements for that badge. Each badge application is reviewed and either approved (with the badge being issued) or denied (with feedback provided on how to resubmit successfully).
While the certification program requires the applicants to make their own connections between the work being submitted and one of the NADSP competencies, each badge is tied to particular direct support skills, with writing prompts provided to help the applicants focus their application on the specific skills and values that reviewers will assess.
The E-Badge Academy will start with 29 badges, but plans have been made to increase the number of available badges at regular intervals. The first wave of badges is tied to the NADSP Code of Ethics, NADSP-accredited training for DSPs, and the NADSP Competencies for DSPs. Future badges will also connect to the National Frontline Supervisor Competencies and the competency statements for NADSP specialty areas.
Going forward, NADSP will offer both the traditional certification program and the E-Badge Academy. These two programs represent two parallel paths which arrive at the same destination, a DSP who has demonstrated the knowledge, skills, and values to provide high quality support.
personal story
Witness to an Epiphany:
Observing DSPs Through the NADSP Credentialing Journey
As a skills mentor and facilitator of the NADSP credentialing process for Direct Support Professionals (DSPs), I have the honor of witnessing epiphanies. As DSPs go through the rigorous credentialing program, there are three aspects of their experience that are universal: They start with initial fear and concern, move into sharing of mutual aid, and emerge at the end in a moment of triumph. It’s my observations about that journey to attaining this gold standard certification that I’d like to reflect on for a moment.
"The only thing to fear is fear itself" (Franklin D. Roosevelt)
The first thing I notice is the initial fear and hesitancy that occurs when a DSP makes the decision to embark on the credentialing path. Many are concerned about the number of training hours and the rigor of creating work samples that illustrate their competency in any of the 15 NADSP DSP Competencies. Usually, with a little coaching, hand-holding, and encouragement the credentialing candidates begin to see that they are able and equipped to proceed. One remarkable thing that happens almost every time I witness this process is that DSPs begin to link what they have been doing in their practice for years to the individual competencies. For example, if a DSP has been in a support role of working with people through crisis and trauma, they can easily connect the Crisis Intervention and Prevention Competency and set of skill statements to what they have been doing for, perhaps, years. When they make this connection there is often a moment of renewed confidence and validation. This is a wonderful thing to see.
All in the Same Boat
The second thing I witness is the use and experience of "mutual aid." The best practice for DSPs going through the NADSP credentialing process is that of being part of a learning cohort. This is usually done by assembling all participants in regularly scheduled group meetings. Each person that is working on work samples and taking related coursework is exposed to others on the same journey. When this is facilitated properly, what occurs is nothing less than beautiful to behold. Learners who are meeting regularly and making connections discover that they are all "in the same boat." They learn from each other, they challenge each other, and ultimately support and validate each other. I have witnessed DSPs who were on the verge of giving up and quitting suddenly be consoled and pushed to continue with their credentialing process by their learning cohort colleagues. I have seen countless times when learners offer advice and suggestions in and around the work sample development process. It is gratifying to step back, as a facilitator, and let the cohort members teach and support each other. There is magic when DSPs listen to and share with each other about their successes, challenges, and love of the practice of direct support work.
Epiphany and Credential
The final stage of this process is the submission of the learner’s portfolio to NADSP. This is a moment that is loaded with anxiety, relief, and celebration. Often, DSPs will say that they aren’t sure they will achieve the certification and they are nervous about sending in their completed portfolio. However, when that moment is facilitated in a way that allows for the DSP’s anxiety, yet confirms and validates the great effort that has been expended and the accomplishment achieved, it can be a great defining moment. About 90 days after that submission results are obtained. From my vantage point, I have seen DSPs cry, cheer, jump around, and gaze into the ether! All reactions are earned, expected, and suited to the efforts that have been painstakingly performed over the past 12 months. When a DSP learns that they have obtained a national certification from the National Alliance for Direct Support Professionals they will generally be numb, and then they will erupt into a great celebration! I have had the honor to observe this and it never, ever gets old. To see DSPs be recognized as professionals is as close to ecstasy as can be. Once the initial joy is felt by the recipient, then comes the best part. It is the "epiphany." I call it that because I have enjoyed the moments when DSPs achieve national certification and then realize they are part of a movement. When a DSP understands that they are valued, skilled, competent and part of a workforce that is responsible for promoting and supporting the civil rights of people with disabilities, there is a moment of triumph and epiphany. Epiphany as defined by Webster’s dictionary is "a moment of sudden revelation or insight." I have been there. It is an honor and gift to see it.
program profile
Maine’s Workforce Challenges:
One Agency’s Attempt to Recruit, Support and Retain Staff
OHI is a nonprofit agency with services in six rural counties. We provide a wide variety of supports for over 600 people with intellectual and/or developmental disabilities (IDD) or mental illness, and to many who are homeless. Like most states, Maine providers are faced with looming workforce shortages that are getting worse.
Maine is the largest state in New England with a population of 1.3 million people, larger than the other five New England states combined. Its unemployment rate is 3.7%, and the rate in Penobscot County, where the majority of OHI employees reside, is 3.1%. Maine’s household poverty rate is 14.90%, the highest of all the New England states. Maine has the oldest median age in the country at 44 and it is getting older faster than any other state. The living wage for a single adult who is working full-time is $15.66 an hour. OHI’s starting wage for a Direct Support Professional (DSP) is $10.50 an hour. These demographics, combined with the rural nature of Maine and the transportation deficits, add up to a significant workforce challenge.
Obviously, the workforce crisis has not left OHI’s DSPs untouched. Fifty DSPs in dire financial need have turned to our Human Resources staff this year in search of help — an unprecedented number. Of 270 DSP positions, we have 63 full-time openings at this time, which is 23% of our full-time positions — more than any time in our 38-year history.
Though the need for qualified employees is ever looming, OHI is taking an alternative approach to assisting employees who assist others by taking the term "benefits" to the next level. Due to their low hourly wage many of OHI’s employees are eligible for many of the same benefits to which individuals they support are entitled. When new or existing employees meet with OHI’s Human Resources Department, it is not only to discuss typical benefits such as medical, dental, and life insurance or how many paid holidays employees receive. It is also to receive information and assistance about other available benefit programs, including government programs.
ON THE FIRST DAY OF EMPLOYMENT WITH OHI, EACH NEW PERSON IS INFORMED THAT IF HE/SHE IS ENGAGED IN A FINANCIAL STRUGGLE, THE HUMAN RESOURCES MANAGER IS AVAILABLE TO PROVIDE ASSISTANCE.
The needs of our employees have increased over the last five years. In 2013, our Human Resources manager confidentially met with and assisted 10 employees with a variety of "alternative" benefits such as food stamps, the Department of Agriculture’s Low Income Rehabilitation Loan program, MaineCare (Medicaid), Low Income Heating Assistance, weatherization assistance, rental rebates, and the Children’s Health Insurance Program (CHIP). In 2017, the manager of Human Resources met with 45 employees, and the number in need continues to increase.
On the first day of employment with OHI, each new person is informed that if he/she is engaged in a financial struggle, the Human Resources manager is available to provide assistance. She meets with individuals in a confidential setting and keeps all conversations private. As CEO, I am not informed of who has these conversations. These meetings have successfully resulted in employees acquiring heating oil for their homes, which is a matter of life and death in the harsh Maine winters; some employees tell us they carry a 5-gallon can in their car and fill it up with heating oil so they can be warm that night. Other employees tell us they have to choose between buying oil and paying their electric bill or buying food for their children. We provide individuals with the address of their local food pantry. We also have a food pantry that some staff patronize, just as people we support and other community members do. There are times when our HR manager goes to a local pantry to pick up food and hygiene items for an eligible employee because of the stigma the employee feels related to "taking charity." Many employees can’t afford the co-pay for health insurance and are unable to pay hospital bills. We work with people to access grant dollars from these hospitals to help pay for enormous outstanding medical expenses.
We find that when we are able to assist and alleviate our employees’ stressors outside of work, they are able to focus more on their roles as DSPs. Employees are more apt to have a deeper commitment to OHI and the people they support because they see and feel that OHI cares about them completely, both at work and outside of work.
We believe that when we intentionally "pay it forward," in this case by assisting our employees with their personal struggles, they will "pay it forward" to others. We see employees we have helped "paying it forward" to their co-workers, people they support, and their families.
Recently, the supervisor of our Human Resources Department was approached by a local philanthropist who had been told about the quality of the department and the services it provides. He and his wife have established a "Pay it Forward" program. They personally identify non-profits whom they think will carry out their "Pay it Forward" practice. Once they are convinced of a successful non-profit’s track record and commitment to "paying it forward," they personally grant money with no strings attached, only asking that the non-profit very intentionally use the money to grow this philosophy — in the belief that this will have a ripple effect.
Through multiple meetings with our leadership team and board and after submitting a proposal about how we would use his money, he made the decision to start giving us money, with no specific limitation. Our proposal accepted by our new friend was to pay forward to OHI employees in need by giving them money to assist with unexpected financial needs. Our proposal included detailed protocols about how we would conduct the program on behalf of our employees with the expectation that we would have an intentional conversation with recipients about paying forward the gift we give to them. This generous philanthropist has given us the ability to increase our support of many desperate employees who may, as the result of his generosity, remain with OHI for years to come.
personal story
My Work is My Life, My Passion
I have been a Direct Support Professional at OHI for 11 years. During the first two years I was working full-time awake overnights at a residential treatment center and part-time for OHI for a day-and-a half live-in…sometimes more!
I live in Lakeville, Maine, population 105 — a 75-mile drive from OHI. During those first two years I had many personal challenges combined with stressors of my full-time job. Among other things, I had been institutionalized for six weeks in a psychiatric facility, where I met my husband. We were married and later divorced. The effects of mental illness, PTSD, divorce, working with young women with borderline personality, and other factors resulted in my doctors recommending that I leave the full-time position.
They asked me to complete an application making a request for a determination of total disability. They said that I could not work then and would never work again. My work with people with disabilities is my life, my passion! I knew that if I couldn’t work, life was over for me. It would be the reason I would just give up and make another suicide attempt. I was not giving up!
I was ready to work for OHI full-time because I really believed in its mission. Unfortunately, OHI’s health plan, in addition to the employee co-pay, didn’t cover mental health benefits and medications that I needed to stay well. Also, OHI paid $4.50 less an hour than the multi-state for-profit. I decided to work full-time for OHI and take this huge pay cut. I was determined that there had to be a way to maintain the health benefits I had and still go to work at the place I really loved.

Gina Russell (right), OHI DSP, meets with OHI’s Human Resources Manager Twila Illingworth Tomlin to talk about the Medicaid program that has helped Gina to continue to work and be well.
Thinking positively, I made an appointment with the Medicaid office. It turned out to be a wise decision. A wonderful worker introduced me to the Maine Medicaid Program for the Working Disabled. I applied and was accepted! This program pays for ALL of my health care and medications. My doctor has to recertify me annually and I have to give consent for the state to review my records. I’m not able to net more than $2500 a month and I have to submit two paystubs as part of an annual redetermination audit.
In addition to this benefit, one of the greatest benefits OHI offers its employees is supervisory support, incredible flexibility, and compassionate understanding. On average, I work about 55 hours a week of live-in because of our terrible workforce shortage. I would work more if it wouldn’t make me ineligible for Medicaid. There are times, though, when I know that I am not feeling well mentally and I have to take a day off. My supervisor is very aware of my mental health and bends over backward to accommodate my request. Our HR manager has assured that I get Intermittent Family and Medical Leave Act (FMLA) coverage when I need to and I never have to worry about losing my job.
The Medicaid program has helped me beyond belief and has allowed me to continue to work while getting the mental health services that I need. Knowing that OHI’s Human Resources Department is always looking for new resources to share with DSPs who need financial and other resource support, I made an appointment with the HR manager to describe the Medicaid program I use, hoping that she would be able to share this resource with other eligible DSPs. Lo and behold, as soon as she learned of this fantastic resource, she shared information about it with other DSPs. At this point, two more DSPs have become eligible for and are using this Medicaid program to pay for their health benefits.
I have always believed in helping other people. By sharing my resource with OHI’s Human Resources manager, just as she shares resources with DSPs, I have found one more way I can "pay it forward." In turn, Human Resources has paid it forward to at least two other DSPs and, perhaps, others of whom we are not aware!
OHI nominated me, and ANCOR chose me, to become ANCOR’s 2013 Maine DSP of the Year. I attended ANCOR’s national conference with OHI’s CEO, Bonnie-Jean Brooks. As I received my award I knew again that my commitment to people with disabilities had enriched and saved my life in more ways than one could possibly imagine.
program profile
Speaking Out for DSP Wages in New York:
The #bFair2DirectCare Campaign

In March 2017, the #bFair2DirectCare campaign pressed for inclusion of a living wage for DSPs in the New York State annual budget, bringing the message to the streets through a billboard and rally in New York City’s Times Square. Photos courtesy of #bFair2DirectCare.
Today, a national and state Direct Support Professional (DSP) workforce shortage is clearly occurring, and it’s forecasted to continue and worsen. Agencies are experiencing worker shortages, and some are in a crisis as they struggle to provide individualized, quality supports in the community. As a result, wages have become a top priority in the effort to recruit and retain skilled workers to provide the necessary supports to people with intellectual and/or developmental disabilities (IDD).
Launching a Campaign to Increase DSP Wages
For years the New York State Association of Community and Residential Agencies (NYSACRA) and our members — 200 agency providers of services to individuals with intellectual and developmental disabilities in New York state — have been advocates for DSPs. A variety of strategies have been promoted to bolster the direct support workforce including valuing and respecting workers through regional DSP conferences and award ceremonies, involving DSPs in decision-making on the job, creating a state chapter of the Alliance for DSPs, developing career ladders and credentialing programs, and increasing wages and benefits.
In 2014, Governor Cuomo announced his plan to increase the minimum wage in New York state. In a process that took two years, the governor was successful and the legislature adopted a multi-year, phased-in minimum wage of $15 per hour. While supportive of the increase, NYSACRA and other advocates for providers that support people with IDD worried that the state would not increase rates paid to provider agencies to pay for the minimum wage increases for those workforce members to which it applied. Further, they were concerned about the increased pressure it would put on agencies providing supports if they could not match this higher wage in recruiting and retaining direct support staff.
A coalition of nine organizations in New York launched a campaign to ensure that public funds would support the minimum wage increase in the rates paid to provider agencies. The campaign was titled, #bFair2DirectCare and the coalition included NYSACRA, New York State Rehabilitation Association, The Arc New York, Interagency Council of Developmental Disabilities Agencies, Alliance of Long Island Agencies, Cerebral Palsy Association of New York State, Developmental Disability Alliance of Western New York, Direct Support Professional Alliance of New York State, and the Self-Advocacy Association of New York State. The first stage of the #bFair2DirectCare campaign was successful and the state fully funded the rate increases to agencies supporting people with IDD, for those staff who would receive the increased minimum wage.
Moving to Stage Two
Immediately after the minimum wage increase was approved, the coalition began the next stage of the campaign in June 2016: Getting to a living wage for the direct support workforce. They chose the theme of #300DaysToBetterPay, aiming to influence the governor’s proposed 2017-18 executive budget slated for release in mid-January 2017. The immediate goal was to get $45 million into the proposed budget for a first step toward a DSP living wage. Key to this phase of the campaign was the fact that DSP positions are, for the most part, not minimum wage positions and the state had not provided, over several years, adequate increases to provider agency funding to keep DSP wages in line with inflation, the cost of living, and an improved economy.
The coalition retained the services of public relations consultants to assist with messaging and media presence efforts, an indispensable part of the campaign. Using the Massachusetts Institute of Technology (MIT) Living Wage Calculator, the coalition developed a plan to get to a living wage in a six-year timeframe, advocating for smaller amounts of funding each year ($45 million/year) versus one large sum of money ($270 million in one year). Creating a living wage proposal required regular surveying of agencies within the provider associations to gather demographic, wage, turnover, vacancy, and overtime data by New York regions. The study was updated regularly for comparison purposes and the data showed a steady increase in vacancy and turnover rates.

When January 2017 arrived, the $45 million was not in the governor’s proposed budget. In a press release the coalition asserted, "Governor Cuomo fails to recognize that non-profits provide this service on the state’s behalf and for less than the state can provide the same services. Yet he endorses and perpetuates a state funding scheme that leaves non-profit providers no leeway in paying workers a salary that provides for their families, which is why many direct care workers must work second or third jobs or are tempted to leave the field for better paying jobs in fast food and big box stores" (#bFair2DirectCare Coalition, 2017).
The campaign shifted tactics and focused on the state legislature. The coalition began efforts to garner the support of members of the state Assembly and Senate, asking them to write letters to the governor encouraging and supporting funds in the final state budget to support the living wage request. People with IDD, parents/family members, and DSPs shared their personal stories with the governor, legislators, and major news outlets. Rallies, press conferences, a billboard in New York City’s Times Square, and radio and TV interviews generated significant media attention and support grew.
The campaign got results and the governor was our hero. At the final press conference before the end of the budget year the governor announced the inclusion of $55 million in the budget to support the living wage request. The budget bill passed with enormous legislative support!
Conclusion
The #bFair2DirectCare campaign was successful for many reasons, and among those that were key were:
- Sharing of awesome and authentic stories by the people most important to making the case: people with IDD, their families, and the DPSs who support them.
- Well-positioned public relations consultants using traditional public relations tactics as well as social media.
- Data on wages — crucial to making the case and backed by a well-respected and independent academic institution (the MIT Living Wage Calculator).
We have four more years to go to funding for a full living wage for New York’s direct support workforce. The #bFair2DirectCare coalition continues its campaigning to ensure the higher wages that are needed to recruit and retain skilled DSPs to support people with IDD. Meanwhile, sadly, the workforce crisis continues.
References
- #bFair2DirectCare Coalition (2017, January). Statement from #bFair2DirectCare Coalition on governor’s failure to include new funding for direct care workers in the executive budget.
overview
Self-Directed Services:
Tradeoffs and Benefits for People with Disabilities and Their Families
Self-directed services and supports are a series of approaches that enable people with intellectual and/or developmental disabilities (IDD) and their families to exercise greater control of their supports than would be expected in more traditional services. Broadly speaking, in self-directed supports a state will assign a budget to a person with IDD and then help the individual design a service plan that meets her or his needs within that budget. The person with IDD (and her or his family in many instances) then hires the service providers and purchases the goods they prefer, often with the help of a paid support broker. In contrast to traditional supports in which an agency chooses Direct Support Professionals (DSPs), self-direction puts the authority and responsibility to hire, train, manage, and fire workers in the hands of people with IDD. A fiscal intermediary will typically assist with payroll tasks to be sure that all DSPs are paid accurately and that taxes are withheld as required by law.
There has been rapid growth of self-directed supports since the initial pilot programs in the 1990s. As of the last national study in 2017 (based on 2015 data), self-directed services were available to people with IDD in 42 states (DeCarlo, Hall-Lande, Bogenschutz, & Hewitt, 2017). There is considerable variation between the states in how they designed their self-directed programs. For example, some states have strict caps on budgets for self-directed supports, while other states allow for more robust and individualized budgets. Some states permit individuals with IDD to hire close family members such as parents or a spouse as DSPs, while other states do not allow such hires. Some states allow an individual to purchase a wide array of approved goods and services, while other states allow expenditures on only a small set of pre-approved services. State administrators who oversee self-directed supports often report a difficult balance between wanting to enable individual choice in how a person with IDD uses supports and from whom, with the need to be cautious in using the taxpayer money that pays for self-directed supports.
BY ALLOWING PEOPLE WITH IDD TO HIRE FAMILY, FRIENDS, NEIGHBORS, AND MEMBERS OF THEIR FAITH COMMUNITIES TO PROVIDE DIRECT SUPPORT, SELF-DIRECTION HAS TAPPED INTO NEW POOLS OF WORKERS.
Regardless of program design, self-direction provides individuals with IDD and their families with some degree of control and flexibility in how their needs are met. However, the degree of control depends on the particular program. For instance, in some states, agency-with-choice models have emerged as a hybrid between self-direction and traditional agency-based services; a person with IDD recruits their own DSPs, who then become employees of a traditional human service organization that helps to manage the employee and becomes their employer of record. In this model, people with IDD and their families have less overall control than fully self-directed supports, but can rely on a third party to manage some of the difficult aspects of employing direct support workers.
No matter what model of self-direction is available in a particular state, people with IDD and their families must consider whether self-direction fits their needs. With the flexibility and choice that can come with self-direction also comes a great deal of responsibility. Individuals who self-direct must carefully plan how to use their allotted budget and make smart choices within the often complex rules that regulate self-direction. Individuals with IDD and their families should also consider whether self-direction is the best option for them in comparison to other programs that are available in the state. Particularly if budget caps are low, it may be hard for a person to get her or his needs met by using self-direction. Individuals with IDD and their families should always consider all options before choosing the program that best suits their needs. Ultimately, self-direction may be best for people with IDD and their families who are willing to advocate for their needs, navigate service systems with limited support, use their social resources to find and manage workers, and have a high degree of accountability for how their funds are used.
For people who choose to use self-direction, there are special considerations related to the direct support workforce. One of the benefits of self-direction is that it typically affords people with IDD and their families much more choice of who provides direct support and how support is provided. In most cases, the person with IDD can choose people they already know to provide their support, and in many states (but not all) can assign wages and work hours for their workers. This choice in who provides direct support for a person with IDD can often result in a better match between the individual and their workers than would be expected in agency-based supports. With the person with IDD as the employer, they have more power to train DSPs to meet their specific needs according to individual preferences.
Some people with IDD, as well as administrators who oversee self-directed services for states, also appreciate that self-direction can facilitate a better cultural match between a person with IDD and a DSP. This may be particularly important, for example, when an individual with IDD prefers to speak a particular language or when they have culturally-grounded food preparation preferences. Self-direction enables a person with IDD to seek out support providers who understand their needs, both cultural and individual, and places the individual in charge of advocating for themselves and training staff to meet their specific needs, making for a strong opportunity for self-determination.
WITH THE FLEXIBILITY AND CHOICE THAT CAN COME WITH SELF-DIRECTION ALSO COMES A GREAT DEAL OF RESPONSIBILITY.
Another major impact of self-directed service and supports is the expansion of the direct support workforce. There has been a shortage of Direct Support Professionals for many years, and that shortage has reached a critical level. The reasons for the shortage are many, including low wages, high turnover, inadequate supervision, limited career advancement opportunities, and often a lack of affordable fringe benefits. Also contributing to the shortage are demographic shifts in the United States. The pool of workers that has traditionally worked in direct support is shrinking as they reach retirement age, and there are fewer new workers entering the field. By allowing people with IDD to hire family, friends, neighbors, and members of their faith communities to provide direct support, self-direction has helped to move us beyond the traditional notion of who can provide direct support, and in doing so has tapped into new pools of workers. As self-direction continues to grow in popularity, this organic expansion of the direct support workforce could help to alleviate strain on other parts of the disability service system.
Self-directed services and supports have the potential to transform the direct support workforce and the way in which people with IDD meet their support needs. From an individual perspective, self-direction gives people with IDD more control of their supports, and can help to improve the self-determination of people with IDD. From a policy perspective, self-directed supports have provided a cost-efficient way to address the direct support workforce crisis, which, when brought to scale, could have major impacts on people with disabilities, state service systems, and the economy.
References
- DeCarlo, M., Hall-Lande, J., Bogenschutz, M., & Hewitt, A. (2017). State of the states in self-direction for individuals with intellectual and developmental disabilities. Policy Research Brief 26(1). [Minneapolis: University of Minnesota, Research and Training Center on Community Living.]
personal story
My Self-Directed Life
My name is Santa. I am a 55-year-old Hispanic woman that has cerebral palsy. I have always been an advocate, speaking up for myself, even at a young age. Being able to dictate how I want people to help me in my life is essential. For me, I think it’s important to know yourself, know your likes and your dislikes. That way, you can tell other people who will help you what services are best for you.
Being in charge of your own self-directed services is not an easy task, but it is one of the most important steps a person with a disability will ever take. People that support you will come and go, but after all, it’s your life and you are the only one who is going to live it.
I choose self-directed services because I want to live my life my way. Sometimes, it is not easy, knowing that some providers may think they might know what is best for you, but service providers are only there to help you meet your needs.
People with disabilities need to come to the table not as voiceless tokens, but rather as active, opinionated, and confident participants. For people to take charge of their lives, they need to know their own disabilities and health care needs, and not be afraid to ask questions when there’s something they don’t understand about their issues. They also need to know what medications they are taking and the side effects. People need to be confident and be able to say "I don’t like this medication" and why. Together with people who support them, they can come up with a plan that both parties are happy with and that they can agree on.

"I choose self-directed services because I want to live my life my way," says Santa Perez.
It is also important for providers to listen and talk to their clients, the people they serve. There have been so many times when the provider talks to the person who is in the room for support, and does not talk to their client or patient. The other person may or may not know what is really going on. Out of respect for the patient/client, it is best to talk directly to them.
It’s important to teach our youth about self-advocacy and self-determination at a young age so they can self-direct their own lives as they get to be adults. The more they know about their own disabilities and health care, the better they can self-direct.
I think key is to have a plan for yourself, but always be willing to take others’ advice. The provider(s) and the client need to be a cohesive team, always able to communicate with each other and to bring other people in to help create a person-centered structure.
For instance, I need PCAs (personal care attendants) to support me. By having self-directed supports, I am able to hire and fire my own PCAs. This includes the ability to choose who I want and feel most comfortable with, which is very important because my PCAs are assisting with delicate needs. The reality is not everyone is compatible with one another. I have found that with self-directed supports, the turnover rate is significantly lower and all parties are much happier. I have the flexibility to set my own schedule that fits my lifestyle.
In the past, when the providers made the decisions about staff and sent their own PCAs, I felt obligated to adhere to their rules, and even though they were kind, I did not feel like an equal partner in the care of my life. I feel I’m the expert on me. I can tell my PCAs the best way to take care of me. I know what is right for me. After all, I have been living with myself for 55 years.
I hope that people with disabilities will realize that they have the right to say "no" if the services they are being offered are not right for them. Self-directed services may not be right for everyone, but they may be right for people with disabilities who want to lead person-centered lives. In my experience, self-directed services ensure that services are person-centered. I’m in the pilot’s seat and have the ability to make the important decisions that relate to me. Not to mention, I can proudly say I have the best PCAs thanks to self-directed services.
program profile
It’s a Matter of Social Justice:
Personalized Supports in Maryland

"Now I am independent and can choose what I want to do!" says Crystal Arbaugh, who receives services through SSMD.
Shared Support Maryland, Inc. (SSMD) is 11 years old and provides completely personalized supports to over 100 people with disabilities. The approach and outcomes are a matter of social justice. Our objective is not to run the lives of people with disabilities, but to support people to run their own lives. Those who hire us live in their own homes, alone or with roommates they have chosen. They hire and are in charge of their own support staff, hold jobs that pay a living wage, and spend their time in activities of their choosing. We are one of a few agencies in the country that provides this kind of person-centered, customized support and services.
It is our intent to support people to make decisions for themselves and to live truly self-directed lives: everyone, any level or multiplicity of disability, no one left behind. People we work for tell us that they have never accomplished so much in their lives. It is our mission to foster and grow community connections and relationships, and value the ambitions and real life goals of the people we support by joining in their pursuits and sharing in their successes. In doing so we inspire systemic change.
SSMD's defining characteristic is our ability to balance rigor and flexibility. Because the best life can sometimes be achieved in surprising and unplanned ways, we seek to balance:
- The discipline of person-centered planning with our commitment to be fully responsive to people’s changing needs.
- The dignity of risk with our commitment to what people define for themselves as safe and well.
- Transparency and accountability with the determination to support people in creative ways.
SSMD is unlike most agencies that provide services in the degree of our commitment to personalized supports. The ways in which we carry out that commitment is the key to our being able to do things differently.
We share our values, tools, and practices through training offered to other agencies serving people with disabilities across Maryland and in other states. With our support, and that of our customers, their families, friends, donors and funders, people who many thought could not live full lives of meaning and impact are making decisions for themselves, mastering skills for life and work, and making meaningful contributions to the world around them.
SSMD focuses on areas that are important to people: Quality service delivery, resource development, organizational development, and staff development. We are most interested in the control people have over their services and supports, if people have and can access the right resources to carry out what they want to in life, and moving professionals and the system out of the way so that they are not between the person and what they need. On an annual basis we survey those who receive our services to receive feedback and see where we can improve. Some of the results from the 2016 survey of 90 customers found that:
- 94% developed, or directed the development of, their person-centered plans.
- 83% reported that SSMD supports them having control of their lives, and more believe that SSMD thinks that their having control over their lives is important.
- 100% reported satisfaction in the area of respect and rights. Further, 93% said that their staff are respectful.
- 87% train their staff and 97% have a role in the management or co-management of staff. They regularly have the opportunity to incorporate what is important to them, including the goals and objectives in their person-centered plans, into the day-to-day management of their teams. We believe that these results are directly related to our efforts to support people with personalized recruitment plans and a hiring process directed by the person from hire to management of their employees.
- 100% are employed in paid positions, making at least minimum wage. People and their teams have researched benefits counseling to help maintain benefits while working. At least one person has taken advantage of their employer’s retirement benefits and stock options!
Among the lessons we have learned that may benefit other agencies providing services and supports to people with disabilities are:
- Remember to hire, connect with, engage with, contract with, and collaborate with those who share your values of basic human regard for each other and social justice for all no matter what. When we have rushed, gone against our gut or didn’t do our homework, it has not been the match between our values, staff, and people we serve that we dreamt of. Not everyone has remained a customer or employee of SSMD, but those who truly share the core of our existence have remained close and we continue to partner with them.
- Stick to the neighborhoods you know. When you work in a community you know, you are best able to connect people to the resources with which you are familiar.
- Loneliness is one of the biggest issues we see in our type of work. When someone leaves their family home, a group home, or a facility it can be a step in the direction of creating a life that is full of excitement, challenge, meaningful connections, and growth.
- Stick to what you know. The world is full of generalists, so make sure you are doing what you do best and use your time wisely. Do not make promises to do everything for anyone; let people know you will walk, run, and fight along with them, and that you will engage others along the way.
program profile
Bringing Young People Into the Direct Support Workforce in Ohio
For many students who do not respond well to traditional classroom methods, the future holds a lot of uncertainties. The Ohio Provider Resource Association (OPRA), a trade association for providers of services to individuals with intellectual and developmental disabilities (IDD), saw an opportunity to not only help at-risk students graduate, but to also grow the workforce of Direct Support Professionals (DSPs).
According to U.S. Department of Labor statistics, direct care is and will continue to be one of the fastest growing occupations (BLS, 2018). As the demand for these supports increases, providers must find solutions to ensure that they grow their workforce to match the demand. To address this need OPRA and the Ohio Alliance of Direct Support Professionals(OADSP) developed the Community Connections Career Partnership-Ohio or C3P(O) program, which launched its first class during the 2015-2016 school year.
The Curriculum
C3P(O) is a training and education program for high school students designed to teach about the direct support profession and the IDD field. The curriculum is based on OADSP’s DSPaths Basic Certification, Certificate of Initial Proficiency (CIP), and Certificate of Advanced Proficiency (CAP), a credentialing program offering sequential credentials that teach, reinforce, and build upon the essential skills of a highly qualified DSP.
During their junior year, students work towards earning their CIP, and work toward earning the CAP during their senior year. To enter the program, students apply towards the end of their sophomore year. If they meet the requirements set by the program and the school, they go through an interview process. This process allows program administrators to select students who are committed to serving others. If students meet the requirements and succeed in the interview process, they begin the program at the start of their junior year.
The program combines classroom-based instruction and on-site mentorships with local service providers. In the classroom, students complete the DSPaths curriculum while building a professional portfolio. The program was originally designed to be taught in three-hour timeframes, but schools have some flexibility to adjust the program to fit their school day. At the end of each school year students are required to demonstrate their proficiency in that year’s curriculum by presenting their portfolio to a panel for grading. To receive the credential, students must receive a passing grade.

Brandon (left), a participant in the C3P(O) program, celebrated the birthday of Jeff, one of the individuals with whom he worked during his mentorship with a local agency.
Last year, the Ohio Department of Education approved the CIP and the CAP as "Industry Recognized Credentials," authorizing the curriculum as a pathway to a high school diploma. Therefore, C3P(O) students are working on obtaining their high school diploma while gaining skills necessary for a DSP. OPRA invested in this program as a way to help ease the current workforce shortage while helping students to graduate from high school. By pairing students with providers, it is a stepping stone to increasing the workforce. The students develop a relationship with the provider who mentors them, and the hope is that they will begin their careers as DSPs once they are certified. Aligning this project with provider agencies in Ohio creates a win-win environment. Participating provider agencies have direct access to a pool of trained and credentialed potential DSPs.
The Students
The curriculum is not the only aspect of C3P(O) that makes the program unique. Many of the participating students did not qualify for traditional vocational training programs, either because of low GPAs or poor attendance records, and were placed into a Career Based Intervention (CBI) cohort. For many CBI students, without successful intervention they are at a significant risk for dropping out of school.
During the 2015-2016 school year, C3P(O) had its first class of 12 juniors at a central Ohio high school. Out of the 12 students, all earned their CIP and 10 moved on to the second year of the program, earning their high school diploma and CAP. During the 2016-2017 school year, C3P(O) expanded to three additional high schools across Ohio, adding 36 new students to the program. Another 36 new students and one more high school have joined the program during the 2017-2018 school year. Since it began, the C3P(O) program has grown more than sixfold, enrolling over 80 students. It continues to garner new interest from different districts, and is on track for continued and sustained growth.
One Student's Perspective
Victoria is a modern-day pioneer. She, along with 11 other students at Franklin Heights High School in Columbus, Ohio, made history at the beginning of the 2015-16 school year when they became the first students to be part of the new C3P(O) program. As a student at the end of her sophomore year, Victoria’s Career-Based Intervention teacher told her and the others that they should become a part of a pilot program that pairs the OADSP DSPaths curriculum with an internship with a local provider of services to people with IDD.
"IT’S NOT JUST A PAYING JOB SOMEDAY; IT’S AN OPPORTUNITY, EVERY DAY, TO IMPACT AND CHANGE SOMEONE’S LIFE IN A GOOD WAY." — VICTORIA
"I have a lot of family in nursing, so I thought it would be easy," Victoria says, "but I was in for a surprise (not in a bad way). The first day I started, I was surprised. I had never done anything like this or ever seen the inside of a facility for people with developmental disabilities — it was so new. The first year in the program taught me patience, open-mindedness, hope, integrity, responsibility, and how I could be a benefit to the individuals I worked with. It’s not just a paying job someday; it’s an opportunity, every day, to impact and change someone’s life in a good way. For example, I worked with an individual who didn’t know how to count money and always had to depend on someone else to help him purchase items, so I taught him the value of coins and how to count them. It wasn’t the most successful project, but it’s the patience and determination to help someone to become more independent that matters. I learned as much as he did."
Victoria and the other 11 students completed the class and received their Certificate of Initial Proficiency at the end of their junior year in high school. As a senior, she was one of 10 who returned to the program and received their Certificates of Advanced Proficiency.
"This program has had a meaningful impact in many areas, but none more discernible than academics and school engagement," says Drew Huber, the Career Based Intervention teacher at Franklin Heights. "Academically the students who participate in the program are at-risk, meaning they are short credits and typically have low grades. Being part of the C3P(O) program has changed that. Students are constantly saying, ‘I have never had grades this good.’ Remember, just two years ago these same students failed multiple classes for a year."
"The second aspect is school engagement," he adds. "These students are part of something. People ask where they are going and they get to explain how they are representing Franklin Heights in a positive manner. They are proud of their accomplishments. Parents call me and explain how much their kids talk about the internship at home and say things like ‘I am not going to get in trouble because I need to be at the internship site.’ This program has had a huge impact on my students’ grades and school engagement. I see it every day."
Chabeley, a classmate of Victoria’s, says, "These past two years I have grown so much. I am truly grateful that I have been given the opportunity to participate in this program. Not only did I learn how to properly give people with disabilities a full life, but I learned a different kind of respect for others."
At the end-of-year ceremony when Victoria received her Certificate of Advanced Proficiency, she had these words to say to her fellow classmates: "This was a great opportunity for all of us. We started off in a sticky situation and we washed it away with success! Day in and day out we learned something valuable. We became generous, motivated, honest, cooperative, creative, energetic, empathetic, resourceful, and learned to become a member of a team. But most of all, we built a family. We were a helping hand to each other and we were making a difference."
References
- Bureau of Labor Statistics (BLS), U.S. Department of Labor (2018). Employment projections. Fastest growing occupations.
program profile
New Technology Means New Options for People Needing Supports:
A Minnesota Story
Until recently "supervision," as used in regulatory language, had often been synonymous with having a caregiver physically present, whether the caregiver is family or Direct Support Professionals (DSPs). This fact has been one of the greatest barriers to individuals with intellectual or developmental disabilities (IDD) living more independent lives. But, what if there was a way for caregivers to know when they are needed and when the person is doing fine on his or her own? What if a caregiver could be assured a vulnerable person got home from work on time, didn’t let anyone else in the apartment, never left the stove on unattended, took medications on time, and could check-in for a chat or a question even with the caregiver miles away? And, what if the tools it took to do all these things were affordable? Remote supervision and support offers those possibilities.
Overview
Remote support and the technology it requires is not new, but spreading the word and adapting regulatory and funding rules to take advantage of it has been a slow process. Because "supervision" required the presence of a DSP, funders felt safe tying payment to DSP physical presence, and regulatory language often used "supervision" and "staff " interchangeably. It all worked, for better or worse, until supervision no longer required the physical presence of a DSP. Minnesota has found a way to adapt funding and regulation to use the new technology tools, and it is starting to catch on.
Minnesota identified two ways of funding remote support through the HCBS Waiver:
- Individuals living in their own home (non-provider controlled) where services are offered via a menu of options. In this situation, remote support technology and services are covered under Environmental Accessibility Adaptations. Since the technology is of no use without DSPs or natural supports receiving and responding to information from the technology, DSP 24-hour remote supervision and response is covered under 24-Hour Emergency Assistance in a daily rate.
- Individuals living in licensed provider-controlled housing with services paid for via an inclusive daily rate. In this case a rate calculation system called the Rate Management System (RMS) is used to determine the daily rate. The RMS calculation is based on the person’s needs, including on-site awake staff, on-site overnight sleep staff, and remote monitoring hours of supervision.
Two organizations using remote support technology in Minnesota are Dungarvin and CCRI.
Dungarvin: Alternative Overnight Supervision
Dungarvin is a national organization of privately-owned companies that are dedicated to providing high quality, community-based supports to people with varying support needs. In Minnesota, it first piloted the use of technology for remote support in 2006, and now uses remote monitoring technology in a number of locations. It took a few years of work with regulators and other stakeholders to receive approval for remote supervision as an alternative to on-site overnight staff, as required by regulation. Dungarvin now uses two active staff overnight to provide scheduled cares and respond to call devices in five homes in Minnesota. Staff can get to each house from another within the times specified in each person’s support plan.
Dungarvin currently uses bed, motion, and contact sensors, and a variety of call devices to match each person’s physical abilities. If a person can’t use a traditional call pendant, a button activated by the light touch of a knee, elbow or head will do. Adapted call devices are mounted to beds, wheelchairs, and walls in bathrooms and anywhere else a person might want to let DSPs know they want help. Dungarvin also uses sensors on individuals’ medication cabinets and sensors to prompt DSPs when critical cares are due, helping the busy staff stay on top of things.
The sensors and call devices are connected to robust software managed by Sengistix, a national remote support vendor. Each person’s support team decides the areas of vulnerabilities for which a DSP needs to be notified and respond in person. Individuals at risk of falls or wandering might require a DSP to respond as soon as a person is out of bed, or out of bed and not moving around in his or her room. Each person served decides how and when to use the call device to request DSP attention. All notifications to staff are private, going to a phone DSPs carry to receive and accept responsibility for responding to notifications. The various sensors also track the care actions of DSPs to help verify how quickly notifications are responded to and timing of critical cares, such as medication administration and repositioning.
CCRI: Independent Housing Options
CCRI, in Clay County of western Minnesota, developed the Independent by Design (IBD) program partnering with Sengistix as the technology vendor. For CCRI and Clay County this program is an alternative to traditional 3-4 person homes. By using the same type of technology Dungarvin uses, CCRI staff support a variety of people with a range of needs, each living in his or her own community apartment/home. Each person, with help from the support team, identifies what situations indicate a need for IBD staff to respond and what the expected response is. It might be a phone call to discuss an issue and offer direction, or a DSP going to the person’s home to provide face-to-face support. When appropriate, the technology keeps staff informed of when individuals come and go, take medications, are in or out of bed, have an activated smoke detector, and so forth. The technology is also used to provide reminders and prompts directly to the person, only involving staff if the matter isn’t resolved. For example, if a vulnerability for one person is getting up and off to work on time, a bed sensor can prompt a phone call to the person if not out of bed by 6:30, again at 6:35 and again at 6:40, if not out of bed. If by 6:45 the person is still not out of bed, the system will call the assigned DSP to intervene per the person’s plan. The same can apply to taking medications, leaving for work on time, or any number of activities and behaviors. When someone needs more intense support and education in certain areas, additional hourly supports can be added and adjusted as the need indicates.
The individuals supported by IBD are not restricted to living in group settings to share staff support. They get the interactive support they need when they need it, while living in the place of their choice. When they don’t need direct staff interaction, they are independent and on their own, knowing support is available at the push of a button. The IBD staff are mobile and can be anywhere in a 20 minute radius, helping someone prepare a meal, talking a person through a tough day at work, checking on a person with diabetes whose refrigerator hasn’t opened all day, being where they’re needed when they’re needed instead of sitting around a group living setting waiting to be needed.
Results
Both uses of technology profiled here:
- Allow individuals greater privacy, dignity, independence, and control.
- Extend the reach of DSPs by helping them know when, where, and how to be of greatest assistance.
- Maximize the efficiency of taxpayer resources by reducing wasted DSP time when they are not needed.
- Improve accountability of the services, as a collateral benefit.
To enable these uses of technology the Minnesota Department of Human Services allowed innovation to occur, then worked with providers and advocates to find ways to responsibly adapt funding and regulation to support it (see the department’s policy page titled Monitoring Technology Usage). Regulations that don’t overly restrict providers or teams enable ongoing innovation, and funding that allows flexibility and adequate resources while still incurring overall savings sets up the system for success.
Short videos on these two profiled programs, along with information about planning, implementing, and funding remote support and assistive technology in Minnesota, are available at the Technology Resource Center. This is a multi-year initiative by the ARRM organization to educate service providers, families and self-advocates, case managers and others.
personal story
“It’s Been Good for Me”: Angie’s Story

Remote monitoring technology helps Angie maintain her independence and privacy, while also receiving assistance when needed.
Angie is a soft-spoken woman, but she knows what’s important to her and was clear with her family and support team it was not living in a group home. As noted by the ARRM Technology Resource Center: "Though experiencing health issues that would ultimately require her to need more intensive care, including possible round-the-clock assistance, Angie wanted to maintain her independence and continue to live on her own without being reliant on a staff person constantly in her home. Angie moved into her own apartment supported by CCRI’s Independent by Design program, which helped to identify, implement, and monitor technology solutions to meet her medical and quality of life needs. Along with hourly staff services to assist with household tasks, technology supports provide monitoring and assistance for needs such as waking up on time and medication management." Beth Dykema, a Direct Support Professional with CCRI’s Independent by Design program, recently interviewed Angie about her home and life.
- Beth
- Tell me about what your life was like before you started with Independent by Design?
- Angie
- I lived on my own. I was mostly on my own. I set up my medications, someone called me [in the] morning when it was time to go to work. Someone came to help me with house work.
- Beth
- Where were you living then?
- Angie
- Different apartment in Moorhead.
- Beth
- I understand you had some health issues at the time. Can you tell me about that and what your biggest concern was then?
- Angie
- I didn't always take my medications. My diabetes was up and the shower bothered me. Now I have help.
- Beth
- When you first heard about Independent by Design and CCRI, what did you think?
- Angie
- I thought it sounded like a good idea. I was scared to move.
- Beth
- What types of technology are you using with the Independent by Design team?
- Angie
- I used to have more. I have sensors for my medications box. I have a button for emergencies.
- Beth
- How does the technology and the Independent by Design team help you to be more independent?
- Angie
- I know there is always someone here. Daily staff visits or I get lonesome. I get out more.
- Beth
- Would you recommend using technology and the Independent by Design program to others?
- Angie
- I would, yeah. It is a good system for people to be in the community and not to stay home.
- Beth
- Anything else you would like to add that you feel is important?
- Angie
- If people really want to live on their own and be independent I think it is a good idea. It’s been good for me.
program profile
One Solution to Minnesota’s Direct Support Workforce Crisis:
DirectCourse Online Training
Minnesotans with disabilities, their families, and providers are experiencing a direct support workforce crisis much like the rest of the country. With high vacancy rates and turnover there simply are not enough available Direct Support Professionals (DSPs) with the necessary skills to support full community inclusion. Due to this shortage, providers, families, and people with disabilities struggle to find, hire, train, and retain skilled DSPs. Also, over the last decade, Minnesota has had a number of legislative initiatives, legal cases, and research efforts that are changing the way people with disabilities live. These forces not only influence the way disability service providers deliver their services, but also increase the expectations of Minnesotans with disabilities and their families for a higher quality of support. As DSPs and other care providers move away from the traditional caregiving model, they need quality training in new person-centered skills and competencies. By providing this training, people with disabilities will receive higher quality community-based support, and DSPs are less likely to leave their positions.
The Minnesota Department of Human Services (MN DHS) recognizes the need for quality training for the direct support workforce. As a result, it has made DirectCourse available as a training resource statewide. DirectCourse is a suite of competency-based, online curricula for those who provide support to people with various physical and intellectual disabilities, those with mental health needs, and older adults. It is operated through a partnership between the Research and Training Center on Community Living (RTC-CL) at the University of Minnesota, and Elsevier, a world-leading provider of scientific, technical, and medical information. It is comprised of five content areas:
- The College of Direct Support (CDS)
- The College of Employment Services (CES)
- The College of Recovery and Community Inclusion (CRCI)
- The College of Personal Assistance and Caregiving (CPAC)
- Person-Centered Counseling (PCC)
MN DHS selected DirectCourse as a workforce training solution because it is a research-informed, evidence-based suite of curricula that includes content across different disability service sectors. All DirectCourse content is developed based on nationally validated competencies and skill sets needed by today’s direct support workforce. DirectCourse measures what a learner can do on the job after training, rather than just accounting for time spent in training, and is delivered through a learning management system called Elsevier Performance Manager (EPM). EPM provides easy access to training records and includes features to customize, track, and assess training outcomes, as well as run reports on targeted training outcomes and document learners’ skills.
Minnesota has used DirectCourse to support DSP training needs since 2004. One early adopter was Habilitative Services, Inc. (HSI) in rural southern Minnesota. With services spread across a large region, HSI recognized the value in delivering training online to its scattered worksites. As Brenda Behrends, Education Coordinator at Habilitative Services, observes:
As Minnesota pioneers of the College of Direct Support, we discovered early on how to solve logistical challenges in training our dispersed workforce along with the many benefits it could bring to our organization. DirectCourse, as it is referred to today, has made a huge difference in how we deliver competency-based training to our employees. It has become an integral part of our quest to provide high quality, individualized supports and services.
In 2009 and 2010, there were several legislative directives to standardize disability services across Minnesota with emphasis on outcomes and person-centered supports. These directives led to the decision to expand the use of DirectCourse, making it more easily available and affordable to all licensed providers, people with disabilities, their families, and other supporters. In 2014, MN DHS decided DirectCourse could support the training needs for both large-scale and small-scale audiences, and expanded DirectCourse access to support system reform efforts. Currently, DirectCourse is available to:
- DSPs, supervisors, and managers
- Disability and human services providers
- Lead agency staff
- Partner state agencies and committees
- People with disabilities and their families
There are currently 30,169 individuals in Minnesota who access content at no personal cost. This group includes 4,916 learners from small agency providers, county and tribal nation staff, and other state agencies who do not pay a licensing fee to use DirectCourse for their learners. Medium (serving 10-100 people with disabilities) and large (serving over 100 people with disabilities) providers, however, do pay a small annual licensing fee for access to the curricula.
MN DHS continues to assess training modules for accuracy and effectiveness while also identifying opportunities for adding training to meet new needs. As Alex Bartolic, the department’s Director of Disability Services, notes:
We did a review with provider representatives of all the training requirements in different rules and statutes and compared them against DirectCourse. We concluded that DirectCourse provides a comprehensive, standardized method to train staff, and the management tools for supervisors to monitor progress and evaluate competency. Providers told us this allowed them to use their limited and valuable supervisory time with staff on what makes the most difference in their ability to do their jobs with specific people.
DirectCourse helps support disability system reform in Minnesota by offering competency-based, on-demand training for direct support staff, service providers, people with disabilities, their families, and other supporters and stakeholders. MN DHS continues to expand its use with people and organizations across the state to support the ongoing changes within the disability service delivery system.
program profile
Enhancing Our Training Capacity:
A Minnesota Organization’s Experience with College of Direct Support
For 94 years, Hammer, headquartered in Wayzata, Minnesota, has been working to fulfill its mission of helping people with developmental disabilities live life to its fullest. We are committed to providing ongoing training and development of Direct Support Professionals (DSPs) and frontline supervisors to ensure a stable and competent workforce that is critical to our mission.
For the past five years, we have been using the College of Direct Support (CDS) online training curriculum to complement our interactive online e-learning lessons. Competency-based, on-demand training is important to Hammer. In addition to meeting licensing requirements, as an organization we want to provide a variety of learning methodologies to meet all adult learning needs and preferences.
What CDS Has Offered Hammer
We created "HammerU" to encompass most of the training available to our staff. We have used CDS as a tool to launch the lion’s share of our trainings. The training content available in CDS enhances our online portion of new employee trainings, and keeps all employees in compliance on a year-to-year basis. One example of how CDS supports our training menu is the modules of content developed to meet licensing requirements in Minnesota. These modules have helped us ensure staff are completing required training. The online content in CDS has been stellar, and has helped us to broaden the reach of our training here at Hammer.

Jethro Lloyd is among the hundreds of staff who’ve received training through "HammerU," which includes the online College of Direct Support.
We chose CDS because it offered the right balance of affordability and content for us as an organization when first embarking on the online learning and management system journey. CDS was a standout in providing agencies with the content that meets current industry standards, practices, and requirements.
The majority of comments we receive from learners who’ve used the curriculum relate to the Person-Centered Practice lessons. Our learners have stated that they really enjoyed delving deeper into the meaning and critical processes connected to person-centeredness on the job. The power of shared stories in the CDS content was a highlight for many learners.
How We Implemented CDS to Grow Our Training
It was a two-year process for us to implement CDS, and it included a task force comprised of the Director of Training, program directors, the Chief Program Officer, and Human Resources. Together we reviewed various options on the market, including a thorough review of the CDS training content and its Elsevier Performance Management System (EPMS). Our purchasing of CDS was one part of further developing our organization’s training department. We then hired an in-house System and Learning Administrator. The role of this new position is to facilitate "HammerU," including systems and learning administration of our training on the EPMS. This role also provides support in developing and facilitating training for all employees as end users.
One of the first steps we took in designing our CDS training program was the decision to limit administrative rights and access for all EPMS functions. This has proven to be a wise decision because it has allowed us to provide consistency in tracking training on the EPMS. The "Ontrack" feature of the EPMS has been very helpful, allowing us to track our own events and classes that are part of our blended learning model for all staff, keeping training records in one place. We have also found that the reporting features support tracking learner progress and identify gaps in training.
We did experience a few challenges during implementation where extra support was needed in navigating the EPMS and understanding the user manual. Some of the features did not work in the way we thought they might, requiring us to invest additional time to figure out how to make the learning management system work for our organization. To address some of these challenges the training team focused on learning management systems and instructional design. This allowed us to develop best practices to create learning modules and break down training content for our staff. Recently, we were asked what we would change to improve the learning administrator’s use of the EPMS, and we recommended creating a user manual for administrative functions with instructions and screen shots.
Lessons Learned and Future Plans
The fact that CDS content is based on current trends in the field, fulfills licensing requirements, and is continually updated is a huge support to us as a large non-profit with 550 employees. It gives us the freedom to create and add new online curricula that are Hammer-focused, which only enhances the training and education we provide.
We have learned some lessons along the way. Developing a learning philosophy for our organization is important. We have now embraced microlearning as a practice for learners on the Hammer team. In our field, the DSP has a huge knowledge base to establish if they are new to our service industry. Micro-learning provides the "need to know" material with laser focus on the industry standards. At the same time we never lose the face-to-face class time in our approach, and keep abreast of current online learning standards as well. Building an easily accessible path of learning early on, including prerequisites, is critical to all learners, their trainers, and mentors.
Training has made a difference in staff recruitment and retention at Hammer. Generally, new employees rate our new hire week-long orientation as above average or excellent, appreciating its thoroughness. We also provide a house-specific training with the employee, their direct supervisor, nurse, and colleagues. When employees feel more secure, knowledgeable, and skilled on the job, we not only increase the excellence in support of those we serve, but our retention of solid employees increases as well. As we look to the future, we will continue to develop and enhance our efforts to ensure that our training stays current with e-learning industry standards in the ever-changing world in which we work.
overview
The Direct Support Workforce Crisis:
A Call to Action
The direct support workforce is critical to the quality and sustainability of the long-term services and supports sector in this country for people with intellectual and developmental disabilities (IDD). While demand has never been higher and will continue to grow, the pace at which true solutions to the workforce challenges are being identified, implemented, and evaluated across states is so slow as to be comparatively non-existent. The realities of high turnover, low wages, poor benefits, and higher vacancy rates have been an ever-evolving plague that has become extremely difficult to eradicate. While asking for and celebrating 1-5% rate increases in order to keep up with inflation is important, it is not the solution to the direct support workforce crisis. The bottom line is advocates, policymakers, and their allies have been slow to make identifying, funding, and implementing solutions to this crisis their top priority. Their focus has been on protecting and expanding services and supports for people with IDD. Without bolder and bigger action, the long-term services and supports system is at stake, and the people with IDD who need it to meet their most basic needs are at severe risk.
Radical changes are needed in national and state level approaches to the procurement and development of the workforce that supports people with IDD. Without these changes, we will not be able to ensure the rights of people with IDD to live and work in their communities. There are practices that we know would address the workforce crisis. For instance, small-scale projects funded through demonstration grants have identified possible solutions, but only small investments have been made by federal, state, and local governments so none have been brought to national scale. Most of these efforts were not sustained following initial funding periods.
We need strong advocacy, community commitment, and action to make solutions a reality. We need collaboration, support, and guidance from state and federal government agencies that focus on health and human services, labor, and education. We need them to work with businesses, advocates, and Direct Support Professionals (DSPs) to find systemic solutions that will:
- Ensure that who DSPs are, what they do, and why they are important is known to members of all our communities.
- Improve DSP identity, respect, and recognition within organizations, state/federal agencies, and communities.
- Create an occupational title recognized by the Bureau of Labor Statistics that accurately identifies the direct support workforce.
- Fund the use of competency-based training models that result in credentialed or certified staff, with corresponding wage increases upon completion.
- Develop industry-specific pipeline programs for youth and young adults to gain education and training while in high school, for displaced workers through workforce centers, and for recently retired persons who are looking for part-time work.
- Gather comprehensive data across states on the direct support workforce, including but not limited to DSP and frontline supervisor vacancy and turnover rates, wages, percentage of full-time vs part-time staff, overtime paid in last 30 days, staff-to-person-served ratios, and authorized versus utilized services by people with IDD who are supported.
- Provide specific interventions and strategies for service providers and individuals/families that employ DSPs on how to maximize their ability to recruit, select, and retain them.
- Promote increased use of self-directed services that provide options for individuals and families to recruit, select, and retain their own DSPs (including paying family members).
- Increase the use of technology-enhanced supports that can provide necessary supervision and support for people with IDD without requiring in-person, hands-on staff.
Through the untiring work of self-advocates, families, DSPs, service provider agencies, and public policymakers a largely institutional care system has been turned on its head by developing a myriad of community-based supports and service options over the past four decades. Now we must demonstrate leadership by preserving and advancing the successes of the past, embracing the work of direct support as a true profession, and attracting new generations who seek it as a career. If we are to really meet the needs of people with disabilities, DSPs will need to possess the tools to be effective community builders, possess the skills to work without a supervisor standing next to them, and understand their rightful place as the lynchpin to quality support for people with disabilities in every community in the country.
Issue back cover










