
This document has been archived because some of the information it contains is out of date. (Effective May 2011)
Volume 12 • Number 2 • June 2001
Family Support for Families of Persons with Developmental Disabilities in the U.S.: Status and Trends
This Policy Research Brief was authored by Susan L. Parish, Associate Project Director; Amy Pomeranz, Resource and Policy Analyst; Richard Hemp, Associate Project Director; Mary C. Rizzolo, Graduate Research Assistant; and David Braddock, Head, all with the Department of Disability and Human Development, University of Illinois at Chicago. It summarizes the trends in family support services for families of persons with developmental disabilities in the U.S. based on longitudinal study conducted by the authors. For additional information the authors may be contacted at 312/413-1431 or sparish@uic.edu.
Introduction
Family support consists of services provided to families with a member who has a developmental disability. Services can include home modifications, in-home and out-of-home respite, sibling programs, family counseling, parent support groups, after-school programs, education programs, behavioral training, and essentially any service funded to assist families to continue to care for their child or adult child with developmental disabilities in the family home. Cash subsidy is a particular form of family support where families directly receive cash or vouchers that enable them to purchase the services or supports they need.
Family support developed in the states in the late 1970s, and has continued to expand (Braddock, Hemp, Parish & Rizzolo, 2000). Prior to the advent of family support, the only form of long-term service available in most states was residential care, mainly in institutions and in the fledgling community-based residential programs that were developing. Families and other advocates argued that states were providing the vast majority of resources to serve those in residential placement, and were ignoring the needs of families who provided care at home. In 1977, the 247,796 people in institutions and community-based out-of-home residential settings represented only 9% of the total population with developmental disabilities (Braddock, Hemp, Parish & Westrich, 1996). The vast majority of the remainder were cared for at home, often with no support provided to their families.
The reduction in residential populations of the nation's public institutions in recent decades has been accompanied by the development of community services in most states. Between 1977-98, the number of persons with developmental disabilities in the nation's public institutions declined by nearly 100,000 persons and the number of persons in community residential programs increased by nearly 250,000 (Braddock, et al., 2000). Part of many states' community services development efforts involved providing support to families to prevent or delay the residential placement of children and adults. Family support program development was such that by 1998, spending totaled $736 million for 328,000 families nationwide.
In this Policy Research Brief summarizing trends in family support services across the U.S., our analysis will show that while there has been dramatic growth in family support services over time, this growth has been quite variable from state to state. It will also show that in spite of tremendous relative advances, spending for family support still comprises only a small portion of total state allocations for mental retardation and developmental disabilities (MR/DD) services. We will examine the financing of family support subsidies, and provide recommendations for the future course of policy in this area.
Method of Study
The analysis presented in this brief is based on statistics collected for the State of the States in Developmental Disabilities Project, a longitudinal investigation of expenditures and services conducted at the University of Illinois at Chicago. The data are collected from a direct survey of state MR/DD agencies, who report an extensive array of spending, revenue, and programmatic information. This larger study encompasses the entire spectrum of MR/DD agency-sponsored services, including residential, employment, family support, supported living, personal assistance, case management, and other community services. MR/DD agency staff concluded reporting data for fiscal years 1997-98 in the fall of 1999 (Braddock, et al., 2000).
Results
In the family support component of this study, respondents were asked to identify spending for family support in three categories: respite, cash subsidy, and other services. States were also asked the number of families receiving these services, and the funding sources for family support. For the questions related to family support spending and numbers of recipients, item response rates of 100% were achieved. Item response rates of 80% were achieved on the questions related to revenue sources used to fund family support, with 40 states reporting.
In order to obtain information on the extent and scope of innovation in family support practices across the states, a second survey was conducted. Each state's Developmental Disabilities Council was contacted in January, 2001, to complete a survey on family support in its state. Forty-six states responded.
Family Support Services
Nationwide, family support expenditures in 1998 totaled $736 million. This represented an inflation-adjusted increase of 93% over the 1993 spending level of $381 million. By comparison, total spending for all MR/DD services, institutional and community, increased 23% in inflation-adjusted terms during the same period. In spite of the relatively rapid increase in family support spending, these allocations constituted just 2.8% of the states' total MR/DD expenditures in 1998, up from 1.8% in 1993. The 93% real dollar increase in family support spending between 1993-98 was nearly twice the 49% increase in overall spending for other community services (e.g., group homes, supported living, case management, employment services, foster care, etc.) over the same period.
The number of families receiving family support services increased by 61% between 1993 and 1998, from 203,874 families to 327,681 families. Between 1993 and 1998, the growth in family support across the nation was primarily due to the enrollment of more families in such programs, not because of large increases in spending per family. The average expenditure per family in the U.S. in 1993 was $1,869; in 1998 it was $2,245, a per-family increase of less than 7% in inflation-adjusted dollars. Figure 1 depicts the growth in family support spending and families served during the 1986-98 period. Inflation-adjusted family support spending increased by an average of 18% annually from 1986-98.
Figure 1: Family Support Spending and Families Served, 1986-98
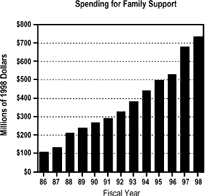
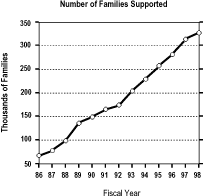
Source: The State of the States in Developmental Disabilities Project, Department of Disability and Human Development, UIC, 2000
In 1998, funding for family support services was provided in all 50 states. Table 1 shows the total spending for family support services for each state in 1998. It shows the percent of total state MR/DD expenditures that were allocated for such services, and also presents data on family support spending per capita (of general state population) and average spending per family supported. The rankings on these latter two dimensions are also indicated in the table.
Table 1 shows clearly that the states varied widely in their expenditures for family support services. Family support spending per capita (of general state population) ranged from $0.09 in Indiana to $12.44 in Arizona. The nation's average was $2.74 per capita in 1998. Eleven states spent at least $5 per capita for family support in 1998, while 16 states spent less than $1 per capita. By comparison, state spending for public and private institutions averaged $26 per capita in the 48 states that funded public or private institutions. Even institutional spending supported only 124,946 residents while 327,681 families received family support services nationally.
An average of 3% of total MR/DD spending nationally was dedicated to family support services. Only five states allocated more than 5% of their total MR/DD budgets to family support initiatives – Arizona, Montana, Kansas, Alaska, and Florida– and 18 states allocated 1% or less.
The average annual allocation per family is another metric by which states' commitment to family support can be assessed. In 1998, the average spending per family was $2,245. It ranged from $129 per year in Idaho to $11,855 in Oklahoma. Ten states spent more than $5,000 per family in 1998, while 11 spent less than $1,000 per family.
Spending in 1998 averaged $2,735 per 1,000 citizens across the nation, and ranged from a low of $85 per 1,000 in Idaho to a high of $12,436 per 1,000 in Arizona. While 11 states spent more than $5,000 per 1,000 citizens on family support services, 16 spent less than $1,000, indicative of the variability among the states in the level of their commitment to supporting caregiving families.
Cash Subsidy Programs
States provided cash subsidies to 20,001 families nationwide, for a total expenditure of $48 million in 1998 (this does not include federal cash payments to families through Social Security Act programs for individuals with disabilities). Families received an average annual state subsidy of $2,416. Twenty-one states provided some funding for cash subsidy programs in 1998. These states are identified in Table 2, along with the number of families receiving subsidy payments, and data regarding the per capita (of general state population) subsidy spending. Cash subsidy spending constituted less than 7% of state's total family support expenditures.
The state with the most generous per-family subsidy payments was Illinois, at $9,110 annually, which was twice the amount provided in North Dakota, the state with the second highest per-family subsidy amount in 1998. Only Louisiana, Oklahoma, and North Dakota were in the top half of all subsidy states for both amount spent per family and numbers of families supported as a percent of their total state population. These three states spent comparatively high amounts per family, but also had programs that reached large numbers of families. The more common occurrence was for states with more generous subsidy programs to subsidize relatively smaller numbers of families. In Illinois, Iowa, Nevada, New Jersey, Oregon, Rhode Island, and South Carolina relatively generous subsidy amounts were provided to proportionately limited numbers of families.
Michigan has been the acknowledged leader in the nation's cash subsidy efforts for many years. The Michigan program was initiated with the 1983 passage of the state's Family Support Subsidy Act. This law provided monthly payments to families with children with severe disabilities, whose family incomes did not exceed $60,000 per annum (Act No. 249, Public Acts of 1983). The program was explicitly intended to reduce out-of-home placement of these children, and ongoing evaluations of the program by the state have indicated that it has been tremendously successful (Michigan Department of Mental Health, 1991). Twenty-five percent of all families receiving cash subsidies in the United States in 1998 were from Michigan. In 1998, the state spent an average of $2,600 per family for 4,936 families, and Michigan's per capita spending for cash subsidies led the nation at $1.31 per state resident.
Forty states reported funding sources for family support services (Table 3). Federal Home and Community-Based Services (HCBS) waiver funds comprised 28% of the resources allocated for family support services in 1998 among the 40 states reporting funding sources. Eleven states did not utilize the HCBS waiver to fund their family support programs, while 11 states relied on the HCBS waiver for at least 50% of the funding of their programs.
Partial correlation analysis showed that controlling for state population, there was a strong relationship between states' use of HCBS to finance family support and their per capita spending for family support services (r=.71, p<.001). These results indicate that states that use HCBS to leverage federal resources have been able to develop stronger family support programs.
Most states' initial programs of family support consisted of respite services and, for some, cash subsidies. By reaching beyond the traditional family support boundaries, states have developed innovative methods of providing family supports.
Innovation in Family Support
To stimulate the development of innovative family support services, the Administration on Developmental Disabilities has provided grant funding to states since 1998 to assist in planning and developing programs of family support. Table 4 provides a list of the currently-funded projects, most at the level of $200,000.
The survey of Developmental Disabilities Councils revealed an array of new initiatives within different states. We have characterized these initiatives within 13 categories:
- Development of a Family Support Policy or Advisory Council: Nineteen states reported they developed a Family Support Policy or Advisory Council in their state. Usually comprised of at least 51% parents and consumers, the advisory council's priority is to serve as the formal mechanism for parents and advocates to have input into family support policy decision-making.
- Self- or Family-Directed Supports: Fourteen states reported programs directed at giving families decision-making authority over the services they receive. Goals of these initiatives include empowering families, and devising family-driven support systems.
- Training, Technical Assistance, and Technology Utilization: Ten states reported training and technical assistance initiatives. The focus of many of these programs is educating service providers, families, and support staff about available services. Some of these states have chosen to use Web-based technology, including interactive Web sites, as a mechanism for reaching people.
- Culturally Competent Services: Eight states reported developing projects to reach minority populations and to ensure services are sensitive to the differing needs of each group.
- Networking/Outreach: Eight states reported using their family support funding as a mechanism to improve their networking and outreach systems to educate and increase communication.
- Integration/Coordination of Services: Seven states reported projects on the integration or coordination of services. These projects include efforts targeted toward developing comprehensive systems, reducing duplication of services, and addressing the needs of individuals missed by the current service system.
- Support to Aging Caregivers: Five states reported that they have initiatives specifically targeted to addressing the needs of aging caregivers.
- Flexible Funding: Twenty-one states reported the use of cash subsidies. An additional five states have developed new subsidy programs that provide families with flexibility and the discretion to determine how their family support funds are spent.
- Policymaking Activities: Four states reported focusing on the development of statewide policy as a mechanism for improving their family support services.
- Waiting List Initiatives: Four states have created initiatives to address the needs of families of individuals who are waiting for residential services.
- Family Support Specialists/Coordinators: Two states reported using specialists or coordinators to more effectively provide family support services. The coordinators can be paid staff or volunteer fami-ly members who assist families secure services.
- Guardianship Alternatives: One state reported focusing their family support services around alternatives to guardianship.
- Localized Service Management: One state reported transferring their centralized services to separate locally managed entities.
Highlighted Examples
To illustrate in some depth the nature of programs underway, we have highlighted three states' programs that address critical family support issues: the needs of aging caregivers, services that are culturally competent, and technology as a method of outreach to unserved or underserved citizens.
Aging Caregivers
The needs of aging family caregivers is a growing challenge for states as the population ages and the life expectancy of persons with developmental disabilities increases. By 2030, the number of persons over age 65 is expected to double to more than 70 million persons (U.S. Bureau of Census, 2001). To address the needs of aging caregivers, the Massachusetts Department of Mental Retardation is collaborating with the Governor's Elder Affairs Office to improve information and increase supports to elder caregivers with a family member with mental retardation. By gathering and analyzing information collected through surveys and focus groups, regional training sessions are being implemented. The sessions increase awareness of the needs of elder caregivers, provide information and resources, share successful strategies on collaboration, and encourage the development of local partnerships. Collaborative activities are underway to strengthen the relationships among community agencies. Additionally, flexible funding has been established to help elder caregivers plan for their family member (Massachusetts Developmental Disability Council, 2001). Other states reporting that they have prioritized the needs of aging caregivers include Idaho, New Hampshire, Ohio, and Pennsylvania.
Diversity
In addition to an increasing number of aging care-givers, the nation's ethnic and cultural diversity is also increasing. The U.S. Census Bureau (2001) estimates that Hispanics currently represent 12% of the overall U.S. population, and will increase their number to 24% in 2050, and 33% by 2100. People of Asian origin currently comprise 4% of the population, and they are estimated to grow to 9% by 2050 and exceed 13% by 2100 (U.S. Census Bureau, 2001). Every culture has its own perception of disability, notions of family,
and decision-making techniques, in addition to using languages other than English, all of which must be taken into consideration when planning and providing services. To address the issues of our increasingly diverse population, Washington state has developed a project to improve services for different ethnic groups. Some goals of the project are to link families and agencies, improve monitoring, facilitate gatherings for families in their communities, and increase the cultural competency of staff through training. The Washington State Developmental Disabilities Council (2000) is the lead agency for this initiative; it has outlined the needs of seven different ethnic groups within the state, and articulated the need for development of services that are respectful of different cultures. Other states reported projects addressing issues of cultural competence, including Illinois, Maryland, Michigan, Minnesota, New Hampshire, New Mexico, and New York.
Utilizing the Internet
Maryland is initiating a project to use technology to facilitate family support outreach. The state's Developmental Disabilities Planning Council has developed an interactive Web site with the intent of promoting family empowerment and family determination. The outreach is being targeted at unserved and underserved families, particularly those from minority backgrounds and those with aging caregivers. The project is also providing technical assistance, training, and public awareness to increase knowledge and understanding of family choices, needs, and supports. This Web site is intended to be family-friendly, and to facilitate resource linkage, use of an interactive discussion group, and other tools to aid families to define and obtain the support services they need (Maryland Developmental Disabilities Council, 2001). As a result of this project, it is hoped that families will report increased knowledge and ability to make informed choices in accessing and evaluating the quality of supports they need. Through the use of the Internet, families who have historically not used or known about family supports will have the opportunity to be more actively involved in the planning, development, implementation and evaluation of the statewide family support system.
Discussion and Recommendations
The overwhelming majority of persons with developmental disabilities are cared for in their family homes, yet state MR/DD resources are allocated disproportionately for the care of those who live in out-of-home residential settings. Advocates have challenged states to remedy the inequity in distribution of services and support. The rapid growth in family support spending during the past decade and a half can be deceptive. While it is true that growth in family support funding has been at a higher rate than that of other sectors of MR/DD spending, this has not resulted in parity for family support with other services. In 1998, states allocated just 2.8% of their total MR/DD resources to family support, even after such spending grew at an inflation-adjusted rate of 93% during 1993-98. While states have clearly devoted more resources to family support, in 1998 family support services were only being provided to an estimated 10% of the population with developmental disabilities.
There are a number of policy recommendations that emerge from this analysis of the existing family support system. Given the primary role of states in funding and directing these initiatives, these are focused on state implementation.
Our first recommendation is that states should aggressively seek HCBS financing to support and expand their family support programs. The HCBS waiver provides an unequaled opportunity for states to leverage their resources and secure extensive federal matching funds for community-based services. Family support can be expanded beyond the means of most states if federal funds are aggressively and planfully utilized to match available state funds.
Second, states should pursue the expansion of programs that invest resources in and facilitate family-directed services and supports. Decisions about what services are needed by families are best made by individual families. Families are the most knowledgeable experts in their own situation and needs. Policies should establish families as the final arbiter of the services that they receive.
Third, family involvement in policy development and oversight of family support programs should be assured. Representative family policy councils should have authority to provide direction to states in the development of services, and families should be integral in quality assurance processes. These roles must be expanded beyond token representation on statewide commissions to positions with authority and decision-making power. Special attention should be given to recruiting leaders from the broad range of families, attending to ages, ethnicity, marital status, and income levels, and meetings and events must be held at times and places that are accessible given families' other obligations.
Culturally appropriate, respectful, and competent supports should be available in all states and from all service providers, and not just through the isolated instances of innovation as is currently the case. The same is true in relation to the needs of aging care-givers. The demographic changes that confront the nation are among the most dynamic forces that will shape our society in the decades to come. It is imperative that policymakers and service providers formulate strategies to meet the needs of a changing constituency of families.
References
- Act No. 249, Public Acts of 1983. Approved by the Governor, December 15, 1983. Lansing, MI: Michigan Legislature. [Michigan Family Support Subsidy Act].
- Administration on Developmental Disabilities. (2000). ADD programs, allotments for FY 2000. Washington, DC: Author, U.S. Department of Health and Human Services. http://www.acf.dhhs.gov/programs/add/program.htm
- Braddock, D., Hemp, R., Parish, S., & Rizzolo, M.C. (2000). The state of the states in developmental disabilities: 2000 study summary. Chicago: University of Illinois at Chicago, Department of Disability and Human Development.
- Braddock, D., Hemp, R., Parish, S. & Westrich, J. (1998). The state of the states in developmental disabilities, (5th ed.). Washington, DC: American Association on Mental Retardation.
- Maryland Developmental Disabilities Council. (2001). NETworks. Baltimore: Author. http://www.md-council.org/resources/family_networks.html.
- Massachusetts Developmental Disabilities Council. (2001). Grants, current grant projects. Boston: Author. http://www.mass.gov/mddc/grants/index.htm.
- Michigan Department of Mental Health. (December 1991). Family support subsidy program: Annual report to the Governor and the Legislature: Fiscal years 1989 & 1990. Lansing, MI: Author.
- U.S. Bureau of the Census. (2001). People, national population estimates and projections. Washington, DC: Author. [Available at: http://www.census.gov].
- Washington State Developmental Disabilities Council (August 15, 2000). Washington state plan October 1, 2000 through September 30, 2003. Olympia, WA: Author.
This issue was supported, in part, by Grant #H133B980047 from the National Institute on Disability and Rehabilitation Research (NIDRR), U.S. Department of Education.
Managing Editors are Vicki Gaylord and Charlie Lakin. The opinions expressed are those of the authors and do not necessarily reflect the position of the Center or its funding sources.
Print copies of this publication are available for $3.00 per copy. An order form is available online, or contact:
Institute on Community Integration University of Minnesota 109 Pattee Hall, 150 Pillsbury Drive SE Minneapolis, MN 55455 612 / 624-4512
Policy Research Brief is available in alternative formats upon request from the above address.
![]()
The University of Minnesota is an equal opportunity employer and educator.
Published on the Web site of the Institute on Community Integration, University of Minnesota (http://ici.umn.edu)
Citation: Parish, S.L., Pomeranz, A., Hemp, R., Rizzolo, M.C., and Braddock, D. (2001) Family Support for Families of Persons with Developmental Disabilities in the U.S.: Status and Trends. Policy Research Brief (University of Minnesota: Minneapolis, Institute on Community Integration), 12(2).